A years-long international collaboration between a hospital in Addis Ababa and Ann Arbor has helped bring new services to the country — and inspire bigger dreams.
1:00 PM
Author |
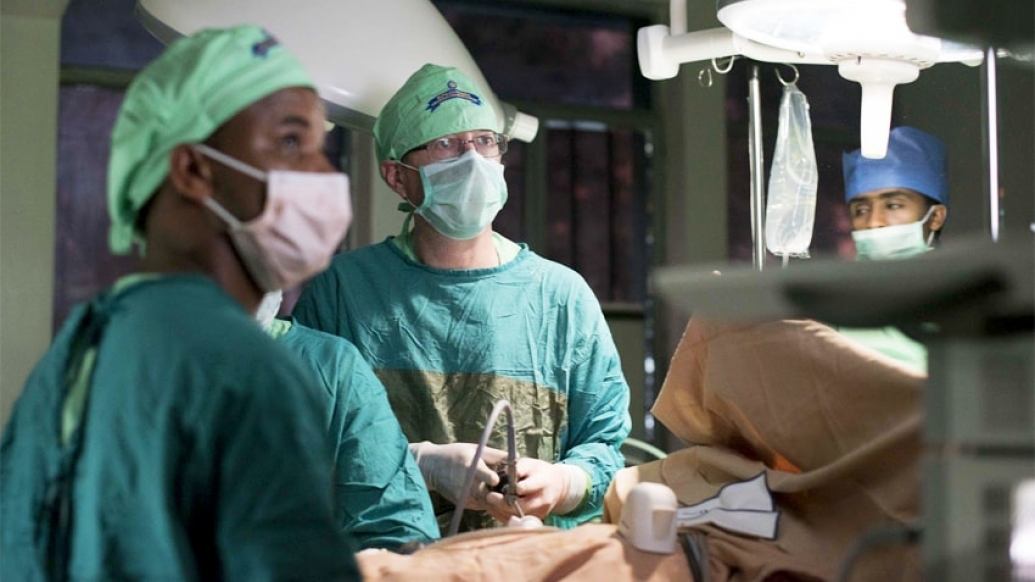
When Momina Ahmed, M.D., was training to be a doctor, she never imagined that she would play a key role in Ethiopia's first kidney transplant.
SEE ALSO: For Kidney Transplants, Timing Is Everything
"As a young medical student, you are always full of energy and you dream — but not of transplants!" she says with a big laugh. "You dream what you know. Back then, we didn't have the theoretical exposure, let alone the practical exposure."
But there she was last September preparing the patient for the historic procedure. Since then, 17 kidney transplants have been done at Ethiopia's new Federal Kidney Transplant Center, where Ahmed is the clinical director.
Only a few other countries in Sub-Saharan Africa perform the procedure. Ethiopia's rapid progress with transplants is one of the best examples of the ambitious and often dizzying reforms in its health care system in recent years.

Laying the foundation
The kidney transplants wouldn't be possible without the capability for dialysis. Ahmed was also the first in Ethiopia to be involved in bringing that function to a public hospital. She does hemodialysis, which involves pumping blood into an artificial kidney machine that filters away toxins before returning the blood to the body.
"I had never seen hemodialysis when I was a medical student or resident. It was difficult to imagine hemodialysis service in a public hospital like St. Paul's," says the physician, who is also head of nephrology at St. Paul's Hospital Millennium Medical College, where the transplant center is located in the country's capital, Addis Ababa.
But perhaps the biggest step toward these capabilities happened about five years ago, when St. Paul's began collaborating with the University of Michigan — a partnership that former Minister of Health Tedros Adhanom, M.D., was instrumental in establishing. As the architect of Ethiopia's medical revolution, Adhanom created a strategy that involved partnering with toptier global institutions with reputations for sticking around for the long term.
The cool thing about the project is that all of the things we're doing are improving the quality of care for everything.Jeffrey Punch, M.D.
The relationship with Michigan began with a program to train doctors in obstetrics and gynecology, an initiative driven by Senait Fisseha, M.D., an adjunct professor at U-M. As the program grew, Fisseha got other U-M physicians involved. One was Jeffrey Punch, M.D., a transplant surgeon.
Before coming onboard, Punch spent time observing Ethiopian physicians operate. He went to their clinics and watched teaching rounds. He was impressed with the surgeons' dedication and shared goals.
"I really got the feeling that the quality people were really swimming to the top, and they were sticking with it," he says. "There was a group of people who could have clearly emigrated and been successful elsewhere, but they were committed to their country, and they wanted to do things."
Punch has been training four Ethiopian surgeons to perform transplants, and he says they might be ready to fly solo in a year or more. Generally, each surgeon will have to do about 20 transplants to be competent.
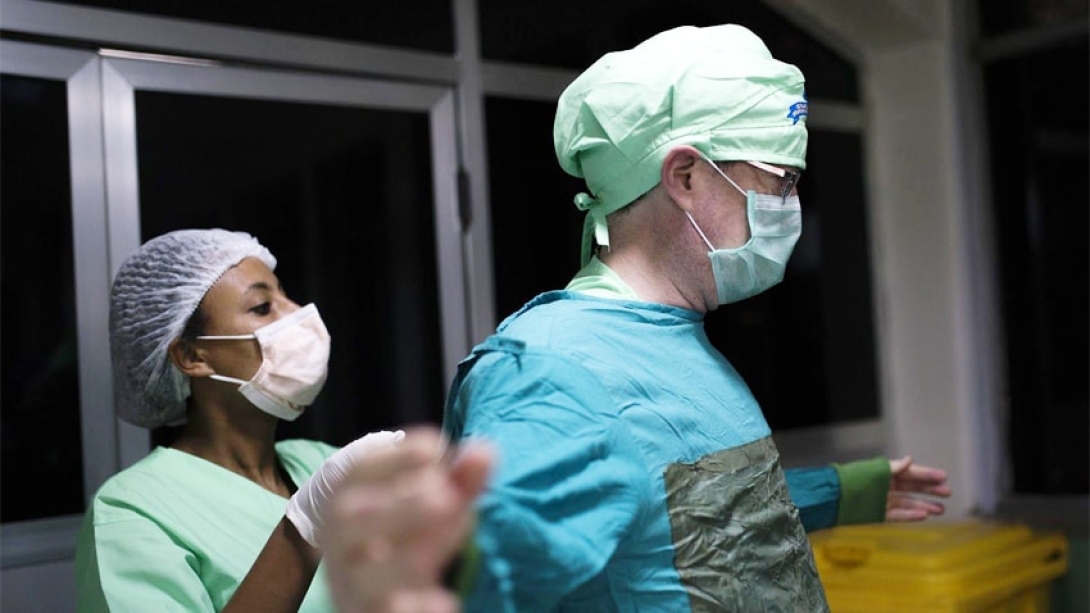
Kidney complications
The procedure is different from heart or liver transplants, which involve removing the bad organ and replacing it with a new one. With kidney transplants, the native organ stays in the body and a new one is added. There's no need to remove the old one because "the badness doesn't spread to the other," Punch says.
SEE ALSO: Will a Kidney Transplant Fail? Genes Could Hold the Key
When the donated kidney is placed in the body, the surgeon must connect it with blood vessels that supply other things. "So you can't mess that up, or they lose their leg or intestines," Punch says.
Critics might argue that something as complicated and expensive as a kidney transplant is not what a country like Ethiopia should be spending its money on. But Punch says a transplant is much cheaper than dialysis and is more effective.
"Kidney disease affects young people in the prime of their lives, and it affects not only the patient, but their family as well," Punch adds. "Losing the breadwinner is disastrous to the family unit. We can see how grateful the entire family is when the patients are restored to health by transplant."
Most people might not appreciate how difficult it is to set up a kidney transplant program. It involves much more than a seasoned surgeon flying in to show other doctors how to do the procedure.
Punch's team spent more than two years working with St. Paul's to sort out a wide range of issues. A variety of drugs and an inventory system to track them was needed. Labs were open only during the day on weekdays, and they were upgraded to be available 24/7. CT scanners, pathology and ultrasound required upgrades. Even new surgical gowns had to be ordered.
"The cool thing about the project is that all of the things we're doing are improving the quality of care for everything," Punch says. "Everyone in the hospital benefits from the fact that they can check all these labs whenever they want to instead of five days a week during the day."
Ahmed says the transplant program is also inspiring doctors in other departments.
"It has motivated other physicians and officials to start thinking it's possible to have new services that seemed impossible before. People are starting to think bigger," she says. "The Ministry of Health is asking Punch if it's possible to start doing liver transplants."
Now they're dreaming what they know.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!