Two hospitalists reflect on caring for one of their own when a very sick critical care physician became one of their first COVID-19 patients.
11:20 AM
Author |
Editor's note: Information on the COVID-19 crisis is constantly changing. For the latest numbers and updates, keep checking the CDC's website. For the most up-to-date information from Michigan Medicine, visit the hospital's Coronavirus (COVID-19) webpage.
Interested in a COVID-19 clinical trial? Health research is critical to ending the COVID-19 pandemic. Our researchers are hard at work to find vaccines and other ways to potentially prevent and treat the disease and need your help. Sign up to be considered for a clinical trial at Michigan Medicine.
They felt a sense of duty and pride volunteering to take care of the sickest patients with COVID-19. After all, this is why Valerie Vaughn, M.D., and Julie Barrett, M.D., became hospitalists.
But when a fellow critical care doctor became one of their early COVID-19 patients, it opened their eyes to what they were really risking. They thought they'd be fine, because they're young. But so is he. They know how to take precautions to keep themselves healthy. But so does he. And yet, he arrived to Michigan Medicine so sick he was being considered for ECMO.
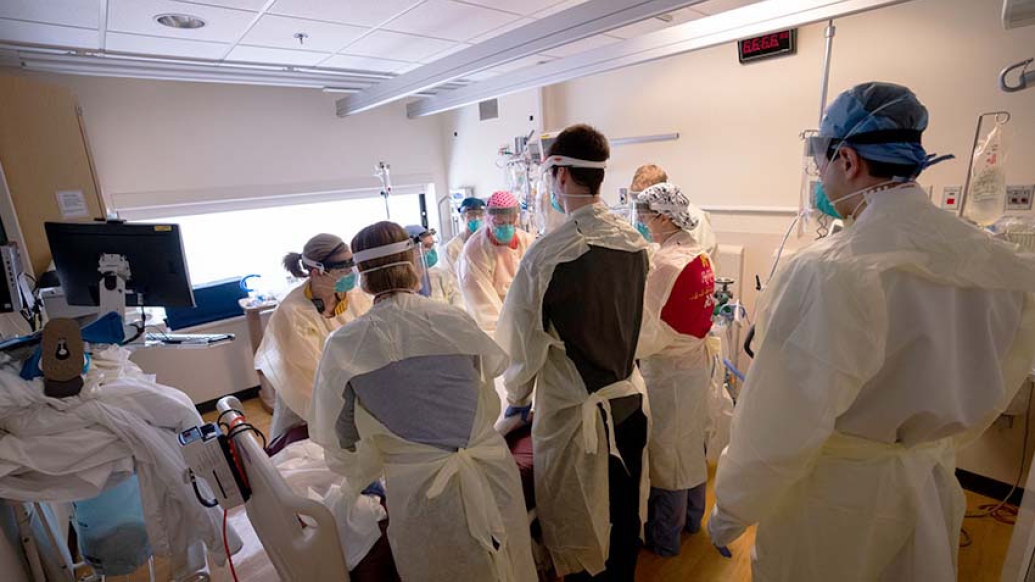
Caring for Detroit physician Eugene Vovchuk, M.D., was a lesson in both medicine and vulnerability for Vaughn, Barrett and their colleagues: from seeing him intubated and put on the highest ventilator setting, to writing his discharge papers and walking him down to his wife's car once his condition improved.
Initial feelings of shock
A few weeks ago, Michigan Medicine got the call about a really sick male patient, struck with COVID-19, who may need ECMO. Short for extracorporeal membrane oxygenation, this intensive care therapy is thought to offer a last chance at life for the sickest COVID-19 patients. Not all hospitals are able to offer the treatment.
He was flown to U-M, and Vaughn and Barrett were ready to help.
"When we realized this was a 38-year-old fellow doctor who was relatively healthy, though, we had two simultaneous thoughts," Vaughn says.
The first was her reaction as a physician to the details of the case: "Oh my goodness, I hope this guy is going to be OK. We have to do everything we can for him." The second was more personal: "We were realizing what we'd gotten ourselves into, and the assumption we'd all had that we were going to be OK wasn't necessarily true. You could just see the look in all of our eyes as we realized it could be us one day."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Barrett was the first doctor to take care of Vovchuk when he got to Michigan Medicine's RICU, the Regional Infectious Containment Unit, which is an isolation unit opened for COVID-19 patients.
"He was intubated and critical when he arrived," Barrett says. "He was on the maximum ventilator setting and he had to be proned," which is a positioning tactic popular in COVID-19 care that involves turning the patient over onto their belly to make breathing easier.
SEE ALSO: 'A New Take on Life' After Recovering from COVID-19
Vovchuk was able to be extubated and continue recovering in the intensive care unit, and then on the general medicine floor. Barrett was there frequently, keeping a close watch on his condition – he was battling delirium – and wielding the smartphone for daily FaceTime check-ins with his wife and young children, who weren't able to visit in person.
"So much with COVID-19 is just time," Barrett says. "In order to be a good doctor, I'm not doing a lot of different treatments every day, but the way I felt I could do something meaningful was connect our patients with their families. I made time for every family member."
From fear to inspiration
She says Vovchuk, who did his fellowship at Michigan Medicine, was a source of inspiration.
"He was the face of all of our fears coming in," Barrett says. "It was still early and I think we weren't realizing how sick people got, how someone otherwise healthy is fallible. All of us taking care of him felt like we could've easily been in his shoes. And yet there's a lot of reason for hope, and most people who are hospitalized for COVID-19 do recover."
"When I volunteered for this weeks ago, I thought: I'm young, I'm healthy, I run miles after work," Vaughn says. "I realized after taking care of Dr. Vovchuk that it doesn't matter; this can affect all of us. Social distancing is important for all of us. I think we need to be really thoughtful about how we stop doing that."
Vaughn says that during this stressful time, every single COVID-19 patient discharge is a victory.
Like Podcasts? Add the Michigan Medicine News Break to your Alexa-enabled device or subscribe for daily updates on iTunes, Google Play and Stitcher.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!