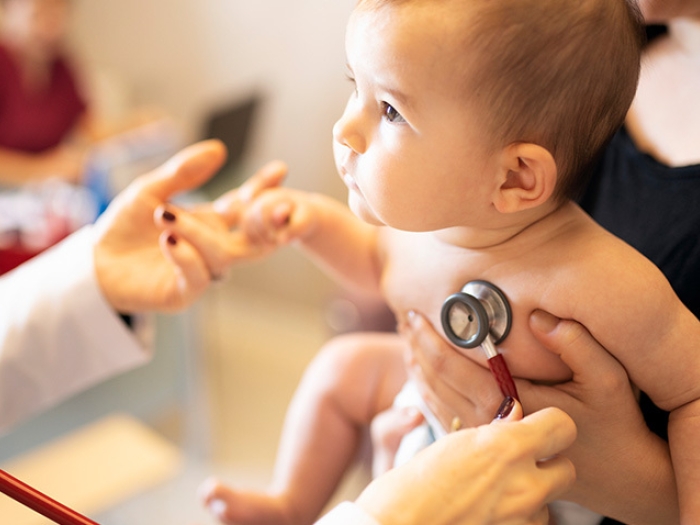
Chest tubes are necessary but painful for babies and children recovering from heart procedures. Doctors explore ways to remove the device earlier to improve families’ experiences and reduce time spent in the hospital.
12:00 PM
Author |
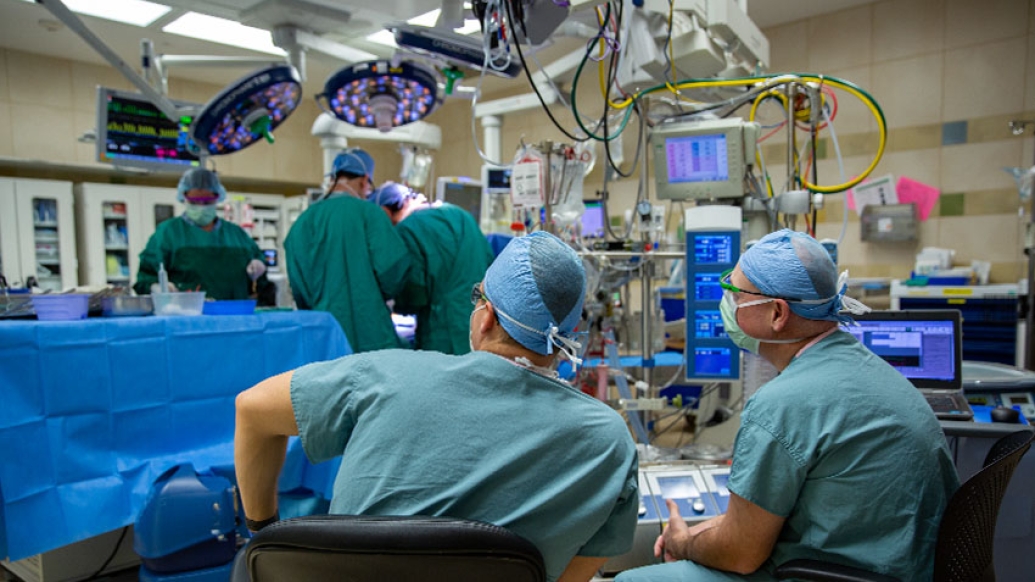
Almost every child who undergoes heart surgery comes out of the procedure with a chest tube, a hollow plastic tube that drains fluid around the heart and lungs and helps patients breathe better.
Chest tubes are critical, but for babies and children recovering from heart operations, they're also painful, uncomfortable, and may delay other aspects of recovery after surgery.
Now, doctors at nine pediatric heart centers have come together to explore ways to limit the amount of time young heart patients have chest tubes in place after surgery.
By learning from centers who removed the tubes early on, and collaborating to share these practices, the investigators were able to reduce children's average amount of time with chest tubes across centers, researchers from University of Michigan C.S. Mott Children's Hospital reported at the American Heart Association Scientific Sessions. None of the centers saw any adverse effects.
Researchers were also encouraged to see that the participating centers saw a reduced length of hospital stay among their pediatric heart surgery patients, down from eight to seven days.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily updates on iTunes, Google Play and Stitcher.
"Chest tubes cause a lot of discomfort, can impact a child's ability to eat and may prolong the recovery process," says lead author Katie Bates, M.D., pediatric cardiologist and researcher at Michigan Medicine's Congenital Heart Center at Mott.
"For older children, having a chest tube means they can't get up and walk as easily. For babies, it means waiting longer to be held normally by their parents. Reducing any time spent with a chest tube benefits all patients and families."
The study included 1,767 pediatric heart surgery patients across participating hospitals, with data collected through the Pediatric Acute Care Cardiology Collaborative (PAC3) and Pediatric Cardiac Critical Care Consortium (PC⁴), two large networks aiming to improve care and outcomes for children with heart disease
The collaboration was supported by Cardiac Networks United, which brings together networks across the field, along with data, expertise, and resources to accelerate scientific discovery and improvements in congenital heart care. These efforts now span more than two thirds of the nation's congenital heart centers.
"Our efforts to remove chest tubes earlier for young heart patients were incredibly successful and a good example of what can happen when centers work together to improve the quality of care for kids hospitalized for heart disease," Bates says.
Collaborating to improve care
Congenital heart defects are the most common type of birth defect, affecting nearly 1 in 100 births.
For the 40,000 children who require heart surgery in the U.S. each year, chest tubes are placed while they're still under anesthesia. The tube is connected to a device to remove air, blood, and fluid from accumulating around the child's heart or lungs.
MORE FROM THE LAB: Subscribe to our weekly newsletter
While there have been many advances in care for congenital heart surgery patients over the last few decades, Bates says, chest tube care is one area that few have evaluated.
"Despite the fact that almost every child who has heart surgery receives a chest tube, there has been almost no research about how these devices are being managed," Bates says.
"Everybody has always done it a certain way without re-evaluating the practice to see if we could improve."
Bates says the effort to reduce chest tube duration started last year when pediatric heart center leaders came together to compare data. Experts found wide variations between their centers, including one center that was successfully removing the devices within a day of the child's heart procedure. Children at this center also tended to spend less time in the hospital.
"When we shared our data with each other, we found that one center seemed to be doing something very different that was working to significantly reduce patients' amount of time with a chest tube," she says.
"After learning how this site manages chest tubes, we challenged everyone to explore a different approach at their own center to remove chest tubes earlier."
For most sites, meeting this goal meant adjusting criteria on drainage volumes used to determine when a chest tube could be removed. But making these changes required close teamwork across multiple specialties, including cardiologists, heart surgeons and nurses.
The abstract received the 2019 Young Heart Outstanding Research Award in Pediatric Cardiology at the AHA meeting.
While the findings are encouraging, Bates notes that there's still a lot of work ahead to both sustain improvement at the participating sites and also share lessons learned to encourage other congenital heart centers to make similar changes.
"For many parents, the day their child gets his or her chest tube removed is a major milestone," Bates says.
"Ultimately, our goal is to help patients get home as early as it is safely possible."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!