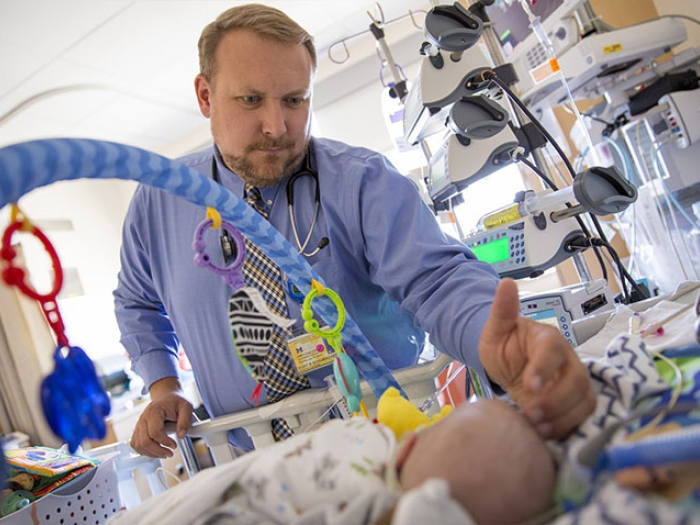
Hospitals around the country collaborate to significantly reduce cardiac arrest rates among children hospitalized with heart disease, according to findings presented at the American Heart Association meeting.
9:45 AM
Author |

Among the most dangerous risks for children with complex congenital heart conditions who are admitted to the intensive care unit is that their heart will unexpectedly stop.
Cardiac arrest increases chances of poor outcomes for young heart patients in the ICU, including high rates of short- and long-term medical problems and death.
Some hospitals are better at preventing cardiac arrests than others – prompting national pediatric heart leaders to come together to figure out why, and how they can learn from the best-performing hospitals.
And within six months of implementing best practices learned from model sites in the country, cardiac arrest rates at the 19 participating hospitals dropped by nearly 45%, according to an abstract presented at the American Heart Association Scientific Sessions.
"We started this research because we thought we could make a big impact on the lives of children we treat in our cardiac ICUs if we could learn to prevent cardiac arrest," says the study's senior author Michael Gaies, M.D., a cardiac intensivist and director of quality at the Congenital Heart Center at Michigan Medicine's C.S. Mott Children's Hospital.
"While some poor outcomes are due to a patient's underlying disease, we know that the quality of our care can improve if we focus on how to prevent arrests rather than how to treat them after they occur. We saw a significant drop in cardiac arrest rates when hospitals adopted elements of care that other hospitals proved were successful."
Dramatic differences in preventing arrests
Cardiac arrest is involved in an estimated 40% of all heart-related pediatric ICU admissions that end in death. Young patients who undergo complex cardiac surgery and patients with advanced heart failure are the highest risk groups.
Most of the current scientific literature is focused on CPR and post-CPR care, not how to prevent the arrests, Gaies says. But by the time CPR is administered, the patient may have already experienced irreversible harm.
MORE FROM THE LAB: Subscribe to our weekly newsletter
Last year, hospitals initiated a Cardiac Arrest Prevention (CAP) quality improvement project to address cardiac arrest rates in the ICU through the Pediatric Cardiac Critical Care Consortium (PC4). PC⁴ unites pediatric heart experts across the country to improve outcomes for critically ill patients with pediatric and congenital heart disease.
Through PC⁴, hospitals were able to share and analyze data about pediatric ICU cardiac arrests across their sites. When hospital leaders compared notes, they found dramatic differences in cardiac arrest rates – with an almost six-fold variation between some children's hospitals after accounting for differences in case complexity.
At some hospitals, a cardiac arrest occurred every five to seven days in the pediatric cardiac ICU, showing that "where you get your care matters," Gaies says.
Experts evaluated what hospitals with the lowest rates were doing better. They found that certain care processes, such as having emergency medications readily available at the bedside at all times, contributed to better prevention of cardiac arrests.
But the best performing hospitals also had something more basic in common: strong communication between nurses and physicians.
"These were not complicated, high-tech practices," Gaies says. "They centered around increasing communication between nurses and doctors in the ICU to recognize who is most at-risk, developing clear expectations about what signs and symptoms might indicate that the patient is deteriorating toward cardiac arrest, and creating a plan to intervene if the patient is getting sicker before an arrest occurs."
Participating PC⁴ hospitals implemented a care bundle used by the most successful hospitals to enhance communication among care teams and better identify and intervene in cases determined to have the highest risk of cardiac arrest. The changes led to a significant drop in cardiac arrest rates.
Implementation efforts were supported by Cardiac Networks United, an organization which brings together data, expertise, and resources across networks to accelerate scientific discovery and improvements in congenital heart care.
The CAP analysis presented at AHA included a cohort of 36,723 cardiac intensive care encounters before the project launched and 4,047 post-CAP. The significant reduction in cardiac arrest rates after implementation of the CAP bundle was most prominent among surgical patients.
"This project demonstrates everything that we envisioned when we created PC⁴," Gaies says. "We collected data to tell us who we should be learning from and participating hospitals willingly shared their knowledge and experiences with each other.
"We then worked together to figure out how to implement changes in practice, and studied our results rigorously so that we could confidently share them with others. We are saving and improving lives as a result of this project."
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily updates on iTunes, Google Play and Stitcher.
Gaies says next steps are to disseminate the cardiac arrest prevention bundle to other cardiac ICUs locally and globally. He hopes that the research helps shift the discussion towards cardiac arrest prevention and leads to more research dollars and time spent on this aspect of care.
"Parents express many hopes and dreams for their child during treatment, but ultimately they want to bring their child home with them. Preventing cardiac arrest is fundamental to achieving that goal," he says.
"Peers in the field who share a devotion to improving pediatric cardiac critical care were able to work together on this project that is positively impacting our patients and their families."
Jeffrey Alten, M.D., of Cincinnati Children's Hospital Medical Center, was the first author on this abstract.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!