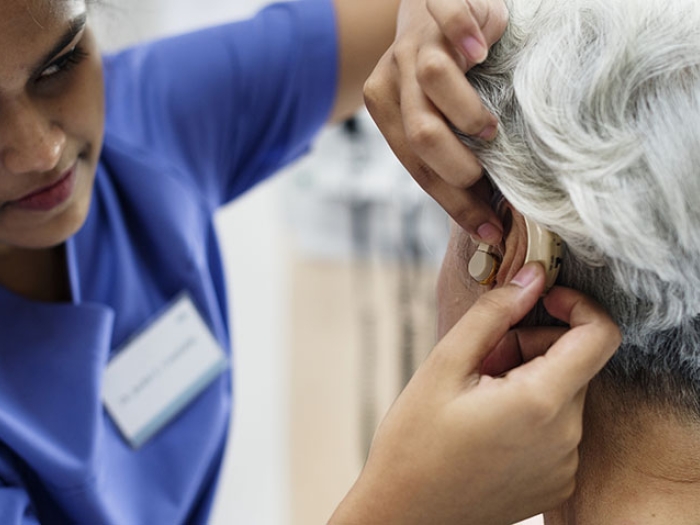
Hearing loss affects about 17 percent of Americans, but screening and referral for evaluation is rarely done. How an electronic intervention may help.
7:00 AM
Author |
Hearing loss is the second most common disability in the U.S., yet it is clinically underdiagnosed.
It's easily identified but is often underdiagnosed by doctors who in some cases wrongly consider it an insignificant issue of aging.
MORE FROM THE LAB: Subscribe to our weekly newsletter
To improve hearing loss screening and treatment rates, Philip Zazove, M.D., professor and chair of Michigan Medicine's Department of Family Medicine, is leading an effort to identify these patients and refer them to audiologists when needed.
"Hearing loss has a huge impact on the lives of those who have it, as evidenced by Helen Keller's famous comment that being deaf is worse than being blind," says Zazove, one of the first deaf physicians in the country. "We know that screening and referral rates for hearing loss are low, so we're focused on increasing them."
Zazove's feasibility study took place at both University of Michigan Family Medicine sites and Beaumont Family Medicine sites. Results are published in the American Journal of Preventive Medicine.
Of the 5,520 eligible patients seen during the eight-month study period, 1,236 patients consented to participate and completed a Hearing Handicap Inventory, or self-assessment of their hearing.
Blinded to HHI results, clinicians received an electronic Best Practice Alert in the electronic medical record to screen for hearing loss during applicable patient visits. Doctors asked patients the single question, "Do you think you have a hearing loss?" and referred those patients who said they did.
At the end of the study, audiology referral rates increased from 1.2 percent to 7.1 percent even though the study was only for eight months.
Overall, 293 consented patients completed the HHI and scored greater than 10, which indicates probable hearing loss. Of these 293 patients, 28 percent were referred to audiologists versus only 7.4 percent with scores less than 10. Forty-two of the 49 referred patients seen by audiologists for which we have information on were diagnosed with hearing loss.
"Our primary findings suggest that what we're doing in these clinics is working," says Zazove. "We are identifying high-risk people and referring them for hearing testing."
Hearing loss has a huge impact on the lives of those who have it, as evidenced by Helen Keller's famous comment that being deaf is worse than being blind. We know that screening rates for hearing loss are low, so we're focused on increasing them.Philip Zazove, M.D.
The impact of hearing loss
Approximately 17 percent of Americans — 48 million — report some degree of hearing loss. The issue is more common in older people, with 1 in 3 people over the age of 65 affected.
Hearing loss is an invisible condition, and the adverse effects on those dealing with it can be feelings of isolation and depression. While the social aspects of hearing loss are well documented, the effects on cognitive development and health have more recently garnered attention.
"We've found hearing loss may be associated with a lot of health problems such as cognitive decline, depression, diabetes, high blood pressure and cardiovascular disease," says Michael McKee, M.D., M.P.H., assistant professor in Family Medicine and co-author of the paper.
SEE ALSO: Second Cause of Hidden Hearing Loss Identified
McKee also has hearing loss and is especially interested in advocating for the rights of deaf and hard-of-hearing patients to obtain equitable health care.
Future implications
While this study significantly increased audiology referrals for at-risk patients, Zazove says larger-scale studies are needed to address the U.S. Preventive Services Task Force's call to assess the long-term impact of hearing loss screening in community populations. He and McKee have begun such a study.
"Making shifts in the health care system can be challenging," says Zazove. "We are making ground, but in terms of what we do once patients are diagnosed with hearing loss, there is still a lot of room for improvement."
Most people who need hearing aids are surprised that neither Medicare nor most commercial insurance plans cover the cost — which can run anywhere from $1,500 to $10,000 per pair. There is often no price negotiation.
"I'm hoping our study will eventually drive some policy change," says McKee. "Whether it's insurance companies covering the costs of hearing aids or helping the United States Best Practices Screening Task Force make better recommendations, it's important."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!