Study shows simple communication tool helps triple the number of babies with congenital heart conditions who experience family bonding before medical interventions.
8:13 AM
Author |
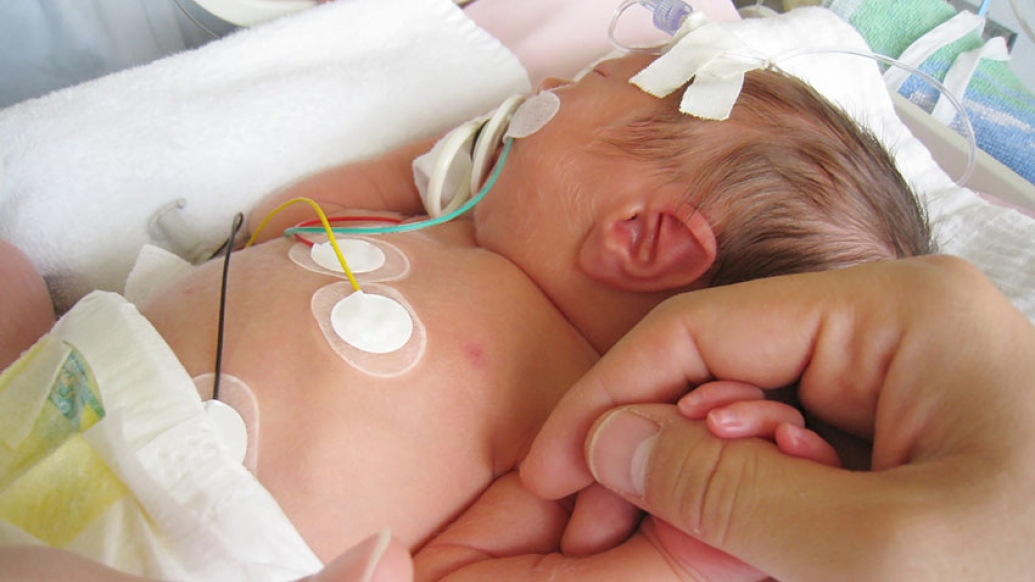
For parents of babies born with heart disease, the first hour with their newborn often means moments full of IVs, wires and procedures to prepare for surgery.
What's sometimes missed in the flurry of medical care is an opportunity for a mother or father to simply hold and welcome their new addition – before their baby is hooked up to any machines.
But a simple tool may decrease unnecessary medical interventions for newborns with certain congenital heart conditions and allow families more bonding time immediately after birth, according to a new study by a congenital heart team at University of Michigan's C.S. Mott Children's Hospital.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
After implementing a new communication strategy, researchers found a decrease in infants who received oxygen or other potentially unnecessary respiratory treatment right after delivery, from 38 to 26 percent. Meanwhile, more newborns experienced maternal bonding time ahead of interventions, from 22 to 74 percent, according to findings presented at the Cardiology 2019 conference hosted by the Children's Hospital of Philadelphia in California.
"Parents of babies born needing heart surgery have a very short period of time when it's just them and their baby, without all of the tubes and IVs and before they get transferred to the pediatric intensive care unit," says Mott fetal cardiologist and study author Sarah Gelehrter, M.D.
"Our goal was to give families more time to snuggle with their baby, take photos and just enjoy those first precious moments. Going from a brand new baby to a cardiac patient is a huge transition and we hope to soften the blow when we can. We found that we could greatly improve newborn bonding time while still keeping the baby safe."
The study included 386 patients from 2005 to 2017 who were prenatally diagnosed with a severe type of heart abnormality called "ductal-dependent" heart disease. Babies with this type of congenital heart disease need medication within their first few hours of life and cardiac surgery before going home. However, they are not expected to be ill right after birth and may appear just like babies without a heart condition. Babies with this heart disease who are not prenatally diagnosed are identified by the state-mandated critical cardiac screening required of all newborns.
The tool researchers used simply incorporated standard language into patients' medical charts, allowing cardiologists to better communicate with the delivery team about the infant's expected course immediately after birth, acceptable oxygen levels, and whether a brief period of bonding was encouraged prior to initiating necessary treatments.
The language was developed by a multidisciplinary team at Michigan Medicine led by Gelehrter and neonatologist, Naomi Laventhal, M.D. The team included representatives from pediatric cardiology, obstetrics, neonatology and nursing.
Mott pediatric cardiology fellow Ian Thomas, M.D., who presented the research at the meeting, notes that caregivers may be prone to providing all babies born with heart disease the same level of respiratory interventions.
"This communication tool makes expectations clear and distinguishes between babies who will likely need immediate intervention after birth from those we don't expect will need any extra oxygen than any other baby," Thomas says
"The language offers the delivery team reassurance that in many cases, allowing families some time together before starting any interventions is OK."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Researchers hope the tool may be considered for babies born with other, non-heart related congenital abnormalities as well.
One in 100 babies are born with a congenital heart disease in the U.S. Within their first hour of life, most of these young patients require an IV to start medication, umbilical catheters, an echocardiogram, continuous EKG monitoring via wires attached to the chest as well as oxygen saturation monitoring through a probe on their hand or foot.
They are then transferred to the PICU in preparation for their surgery followed by a week or more recovery time at the hospital.
"We know that maternal and family bonding can have big benefits for both newborns and their parents," Gelehrter says.
"Everyone wants to make sure we are taking care of these patients in the best way possible. This is a simple way to help more families enjoy the newborn period and normalize what can be a very stressful hospital experience."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!