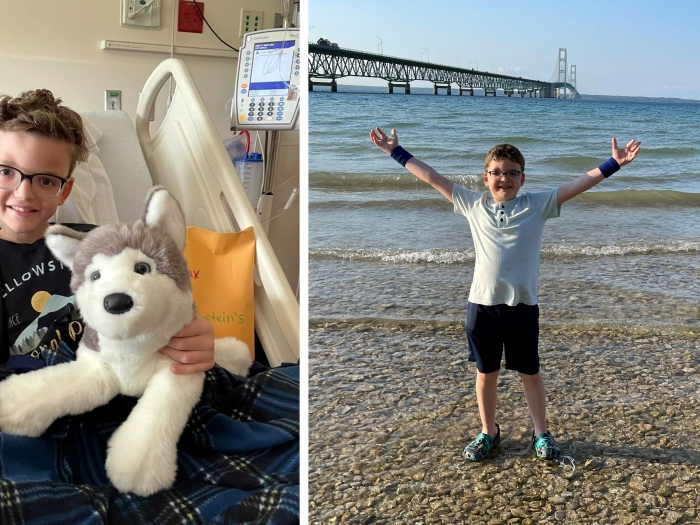
People with medication-resistant epilepsy haven’t had many options. Now, a minimally invasive procedure uses lasers to stop the seizures.
7:00 AM
Author |
It's a disease that can steal the most productive years of a person's life. And for some patients with epilepsy, medications aren't effective. Neurosurgery may not be in the cards, either.
MORE FROM THE LAB: Subscribe to our weekly newsletter
Challenging the status quo that those epilepsy patients must settle for managing seizures instead of stopping them, a Michigan Medicine neurosurgeon is among the first doctors to use a new therapy designed to offer relief.
The method: lasers.
It's called laser interstitial thermal therapy, LITT for short, and it uses a beam of targeted heat to attack — and destroy — the portion of a patient's brain causing the seizures. Emily Levin, M.D., says laser ablation for epilepsy has been an option for only about five years, and few centers offer it.
Despite its newness and relative obscurity, the treatment has potential.
"It's a less invasive procedure, which means the recovery is quicker and it may be a possibility for more patients," says Levin, an assistant professor of neurosurgery at the University of Michigan. "There are a lot of people who have been told they can't have surgery for their epilepsy and they just have to live with it, so they've stopped trying.
"This is a new procedure that can allow those people to have a surgery and, perhaps, a chance to live without epilepsy."
It could help treat other conditions, too. LITT has been used to attack brain tumors such as glioblastoma.
This is a new procedure that can allow [epilepsy patients] to have a surgery and, perhaps, a chance to live without epilepsy.Emily Levin, M.D.
Targeting the trouble tissue
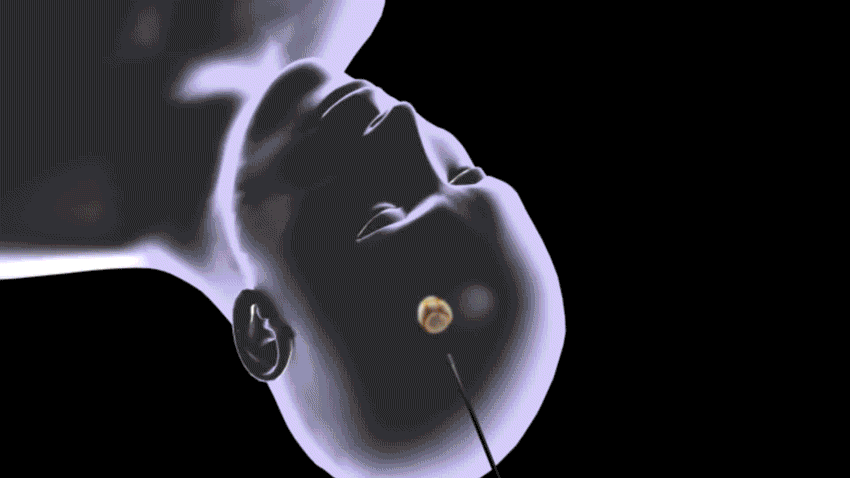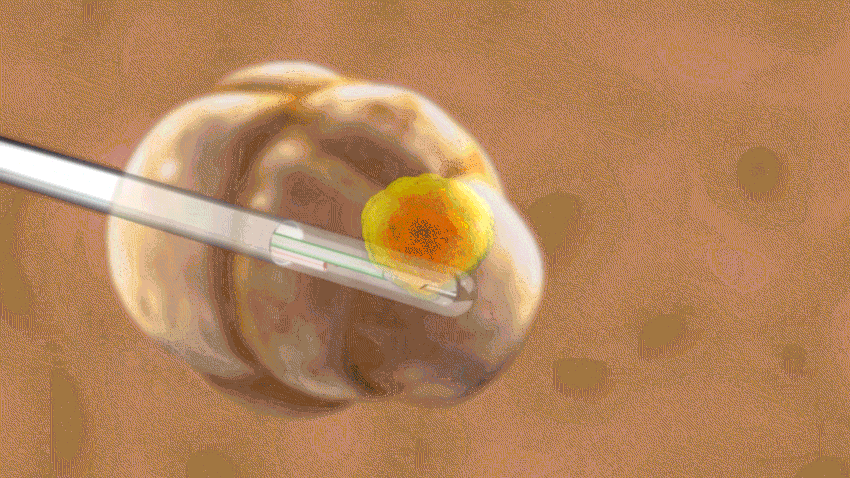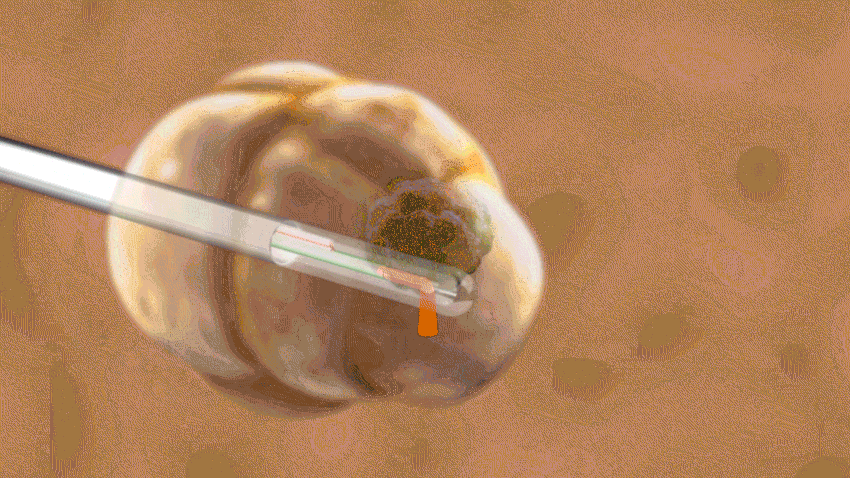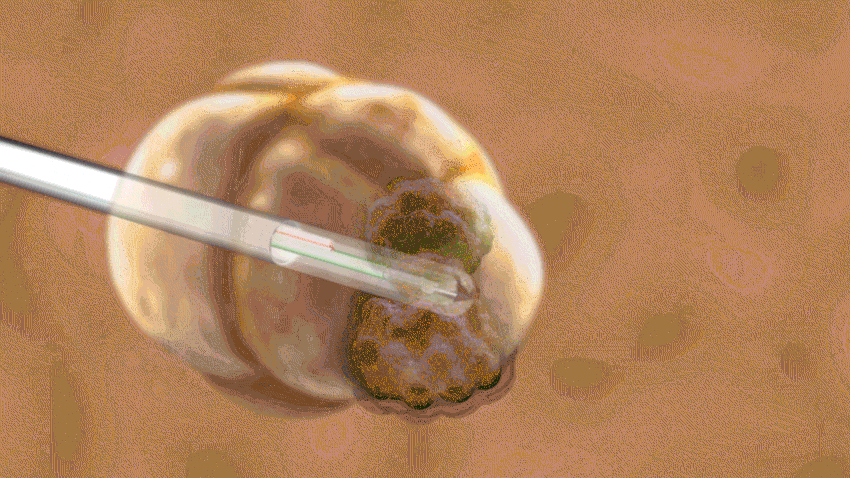
Levin performs the LITT procedure in an MRI suite, using a fiber-optic system called NeuroBlate. LITT starts with a pinhole incision, and then the laser is employed.
Levin goes in with a plan: She has mapped out the precise path the laser will take to target the trouble tissue.
Meanwhile, technical precautions are in place to ensure a patient's safety.
"The laser is MRI-compatible, to monitor the temperature of the brain," Levin says. "Our team watches the heating of the brain along the laser fiber in real time, targeting the part of the brain causing the seizures."
Levin says temperatures typically reach about 50 degrees Celsius (about 122 degrees Fahrenheit). And it takes her just minutes to heat and remove the trouble spot, rather than the hours that doctors would take to remove the tissue during a typical epilepsy surgery.
Carbon dioxide cools the laser along its path so that only the tissue near the tip is affected. Spinal fluid cools and protects surrounding areas of the brain, Levin says.
New chance at relief
Edward Wilkerson was one of Levin's first Michigan Medicine patients to undergo the LITT procedure this summer. Wilkerson's seizures stem from his rare benign congenital tumor called hypothalamic hamartoma, or HH.
SEE ALSO: Fighting Sudden Death in Epilepsy Through Science
"I'm trying to get to where I don't have this problem, period," the 46-year-old says.
After several medications failed and a gamma knife surgery didn't stop all the seizures, his neurologist and neurosurgeon thought LITT was worth considering.
The location of Wilkerson's brain tumor was tricky: It's near the area that transmits memory, called the fornix, and the area that controls body temperature, weight, appetite and sleep cycles, called the hypothalamus.
LITT allowed maximum precision and maneuvering.
"The advantage of the laser is the minimal risk of damage to these surrounding areas," Levin says.
Wilkerson's neurologist, Nusha Mihaylova, M.D., Ph.D., says LITT is gaining popularity at epilepsy centers, in particular for the treatment of HH.
"There are only a few published series of patients with HH treated with LITT, but they show promising results in terms of post-surgical seizure freedom and low rate of complications," she says. "Long-term clinical follow-up of HH epilepsy patients treated with LITT will continue to define its role in the treatment of this pathology."
Life after LITT
Patients recover more quickly with LITT than after traditional brain surgery. This is key for people who need to return to work and other activities their epilepsy may have hindered, Levin says.
Wilkerson went home the day after his procedure and is doing well three months later. Although he has had two provoked seizures, Levin says that his condition is likely to improve — and that LITT may be repeated if necessary.
Adds Mihaylova: "Most importantly, he has not suffered any complications and reports improved quality of life."
LITT provides a much-needed option for patients with HH. For other patients with epilepsy, it offers a less invasive option before others are considered.
"We know the chances of being seizure-free are slightly less with LITT for temporal lobe epilepsy patients, the most common indication," Levin says, "but if someone does continue to have problems, it is possible to perform a traditional surgery later."
Video footage courtesy of Monteris.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!