The in-office eye treatment, now offered at U-M, can help improve outcomes for keratoconus or other corneal diseases.
7:00 AM
Author |
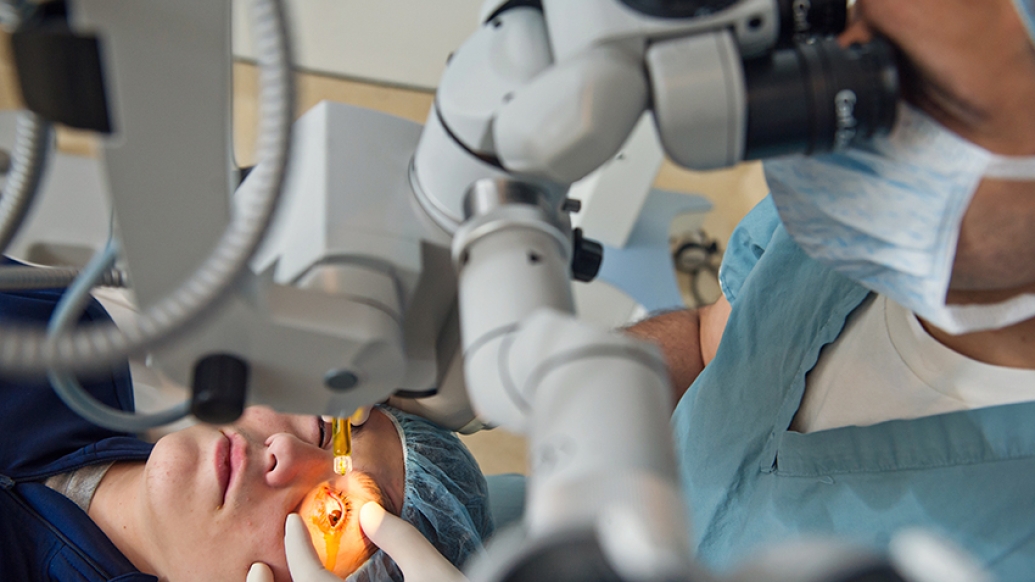
The University of Michigan Kellogg Eye Center is offering a new way to stop progressive vision loss.
MORE FROM THE LAB: Subscribe to our weekly newsletter
Corneal cross-linking is an in-office procedure that strengthens the cornea if it's been weakened by keratoconus, other corneal disease or, rarely, as a complication of LASIK surgery.
What's new and exciting, says cornea specialist Shahzad I. Mian, M.D., is the option to prevent vision loss before patients with keratoconus need corrective lens and, even more significantly, to reduce the need for corneal transplants.
Keratoconus tends to be diagnosed among teens and young adults and progresses for 10 to 20 years before slowing. The earlier it can be treated, the better the outcome.
"Up to now, treatments have been focused on management of symptoms, often with specialized contact lens and, if patients don't see better, then corneal transplants," Mian says. "We can now offer a treatment that, if provided early in the disease, can help maintain better vision."
We can now offer a treatment that, if provided early in the disease, can help maintain better vision.Shahzad I. Mian, M.D.
What to expect from corneal cross-linking
Keratoconus causes the cornea — the front window of the eye — to be distorted and shaped like a cone.
The abnormal shape can cause vision changes, such as light sensitivity, glare and irritation, and can lead to frequent changes in glasses and contact lens prescriptions for nearsightedness.
The cornea contains tiny fibers of protein called collagen, and these fibers help hold the cornea in place and keep it from distorting.
Corneal cross-linking involves removing the front layer of the cornea and administering an eye drop of liquid riboflavin (vitamin B2) to the surface of the eye. Ultraviolent light is then delivered to the eye at differing levels of time and intensity. The eye drop helps the cornea absorb the ultraviolet light and stiffen.
The procedure lasts 60 to 90 minutes. Patients will see results after six months to one year.
SEE ALSO: Evolving Macular Degeneration Treatment Guidelines for Ophthalmologists
Mian and his team helped study which level of treatment is most effective in strengthening the corneal fibers and slowing the progression of keratoconus and corneal ectasia (a condition similar to keratoconus, although it occurs after refractive surgery).
University of Michigan Kellogg Eye Center is among the most experienced ophthalmology programs in the nation to offer corneal cross-linking, also called collagen cross-linking.
Kellogg began offering cross-linking to patients three years ago during national clinical trials to examine the procedure's safety and effectiveness. Results of the trial, which were sponsored by Avedro, a pharmaceutical and device company, led the U.S. Food and Drug Administration to approve cross-linking as a new treatment for progressive keratoconus in mid-April.
The procedure was already available in Europe and other parts of the world.
Outlook for keratoconus
Mild cases of keratoconus can be successfully treated with glasses or specially designed contact lenses. A customizable oversized hard contact lens device called Prosthetic Rehabilitation of the Ocular Surface Ecosystem can also improve vision for patients with keratoconus. In addition, intracorneal rings have been approved to treat the condition.
Earlier this year, Kellogg published findings from the largest ever study of the cornea condition that revealed other hidden risk factors.
It's unclear what causes keratoconus, but theories include genetics and environmental causes.
-
Environment causes: Vigorous eye rubbing is thought to add to the development and progression of the disease; therefore, patients with keratoconus are advised to avoid rubbing their eyes. Many who have keratoconus report having allergies; however, the link to allergic disease is unclear.
-
Genetic causes: Population studies show the condition is more common in the Middle East (perhaps because of dry conditions) and among Indians, Pakistanis and Arabs compared to Caucasians, suggesting a genetic component. Kellogg is helping to investigate which gene causes keratoconus.
Although both eyes may be affected, one eye is usually worse than the other. Patients who had an eye treated during the clinical trial may seek treatment for the other untreated eye — if vision has worsened.
"Those cases demonstrated the effectiveness of cross-linking for slowing the progress of keratoconus," Mian says.
Article photo by Leisa Thompson

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!