Academic research has long been characterized by silos and protective instincts. A new crop of fresh-thinking physician scientists are turning that model on its head, and the results are saving little hearts.
9:49 AM
Author |
More than 1 in every 110 babies is born with some form of congenital heart disease. CHDs are the most common birth defect, in fact. Clinicians have made great strides in improving care for these children, and even individuals with severe diseases may now live well into adulthood. However, not all survive and many still experience significant complications.
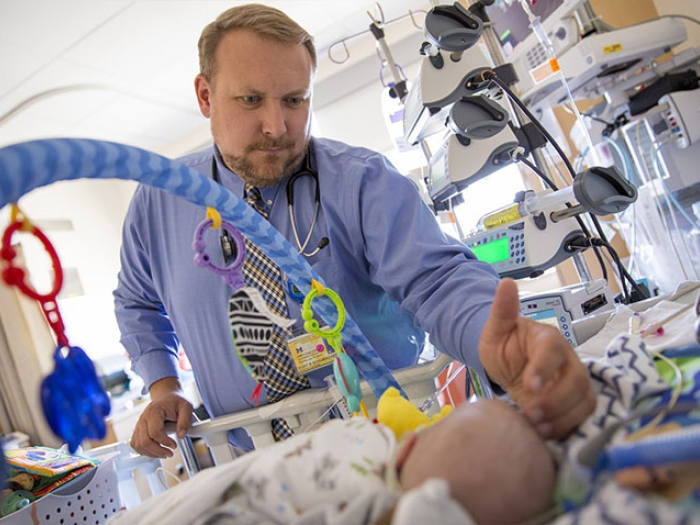
"As a doctor in a pediatric cardiac ICU, we know there are things we want to do better," says Michael Gaies, M.D., a cardiac intensivist and director of quality at the Congenital Heart Center at Michigan Medicine's C.S. Mott Children's Hospital.
"We believe we can improve care for kids recovering from heart surgery if we can better control certain parts of the post-operative journey."
The problem? Data, or rather, lack of it.
"We're a large, experienced heart center with patients travelling here from around the globe, but we knew we weren't going to find the answers by ourselves," says Gaies.
Strength in numbers
By scientific standards, even the highest volume heart centers may not see enough patients with certain types of heart defects to allow in depth study of treatments and outcomes.
Several initiatives had begun to collect information across hospitals for research studies and other purposes, but participating hospitals often only had access to their own data, at best, and opportunities to share information across hospitals and learn from one another were limited. In addition, many efforts focused only on one aspect of care and short-term outcomes, making it difficult to evaluate the broader impact on patients and families, including long term survival, quality of life and need for subsequent care across the continuum of CHD management.
Fortunately, Gaies and his colleagues at U-M weren't alone in dreaming of something better.
In 2009, they created the Pediatric Cardiac Critical Care Consortium (PC4), entering what has become a new era in congenital heart research.
"PC4's work is focused on improving the quality of pediatric cardiac critical care – for example, the care a child might receive immediately after a complex heart operation," notes Kurt Schumacher, M.D., a U-M pediatric cardiologist and director of the PC4 Data Coordinating Center.
Hospitals participating in PC4 commit to sharing data freely, enabling any participating center the ability to better understand care practices and outcomes across the member institutions, and to learn from one another.
I'm not just talking with colleagues across the hall anymore, I'm talking with colleagues across the nation, almost every day. We're all on one team now.Michael Gaies, M.D.
The sophisticated data platform PC4 is built on gives participating hospitals access to real-time, actionable data to support local improvement activities, allowing clinicians and researchers to focus on whichever aspects of care, patient populations, or other variables are of most interest to them.
Early impact
In essence, the Mott researchers and their colleagues took down the walls and barriers isolating hospitals from one another and created a single, state-of-the-art data repository, accessible to all within the network.
"Now a hospital can conclude, 'our outcomes aren't as good as we'd like them to be – what are other hospitals doing that's different?" Gaies says. "What approaches can we study or implement to improve care for our patients, too?"
Conversations like those Gaies describes are already changing the field of cardiac critical care in children's hospitals.
Gaies points to a recent example that illustrates the work they set out to do with PC4. "Cardiac arrest in the ICU – when the heart stops and patients need CPR – takes a lot of lives every year, and permanently alters many others for those who are lucky enough to survive," shares Gaies. "Quality improvement efforts have always focused on what we do after a child has cardiac arrest – which basically amounted to us looking at how well or how quickly we do CPR for the patient. Based on PC4 data across multiple centers, we decided instead to turn our attention to preventing cardiac arrest in the first place."
PC4 researchers could see wide variation across hospitals in how many of their patients experienced a cardiac arrest. The team was able to hone in on what types of patients are at highest risk for post-operative cardiac arrest, and – most importantly – what the top performing hospitals were doing differently in caring for those patients.
The group has since developed and implemented a cardiac arrest prevention bundle across PC4 hospitals.
"Data analysis is ongoing and early results will be presented at the upcoming American Heart Association Scientific Sessions," says Gaies.
We're building an improved infrastructure for research and improvement efforts. The possibilities are infinite.Sara K. Pasquali, M.D.
Expanding reach
PC4 has grown from 6 to 57 member hospitals and counting in the last six years. While the time in the ICU is important, however, the physicians recognized that it is a relatively small part of a patient and family's life with heart disease.
In order to expand these efforts beyond the cardiac intensive care unit setting, PC4 recently joined forces with four other large research and improvement networks, together forming a new initiative known as Cardiac Networks United.
"Cardiac Networks United member institutions span more than two thirds of all hospitals caring for congenital heart patients in the US." says Sara K. Pasquali, M.D., pediatric cardiologist and director of research at the Congenital Heart Center at Mott. "It's allowing us to break down traditional silos and conduct research across multiple phases of care so that we can study and improve outcomes across the lifespan for those affected by CHD."
Pasquali and Gaies co-direct the new initiative alongside Cincinnati Children's Hospital cardiologist Jeffrey Anderson, MD, and they have high expectations for the endeavor.
"We're building an integrated, scalable infrastructure for research and improvement efforts in the field. Cardiac Networks United can connect data collected by a broad range of clinical research and quality initiatives and bring together professionals with diverse areas of expertise to foster greater collaboration" says Pasquali.
Exciting horizons
New published research is starting to churn out of the networks and their member institutions. Cardiac Networks United research has been showcased at the annual Scientific Sessions for both the American College of Cardiology and American Heart Association.
The early success of the endeavor also spurred a partnership with The Children's Heart Foundation, which made a $1.5 million gift to support large-scale research and quality improvement initiatives led by Cardiac Networks United.
"This approach of collaboration and data sharing is really changing the way we do things in the field," says Gaies. "I'm not just talking with colleagues across the hall, I'm talking with colleagues across the nation, almost every day. We're all on one team now. And we're not just making things better for the kids at our own hospitals, or in one part of the country. What we're doing can make a difference for all patients and families battling congenital heart disease."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!