A renowned expert in the field for 40 years discusses the surgical advancements that changed the trajectory of hypoplastic left heart syndrome.
5:00 AM
Author |
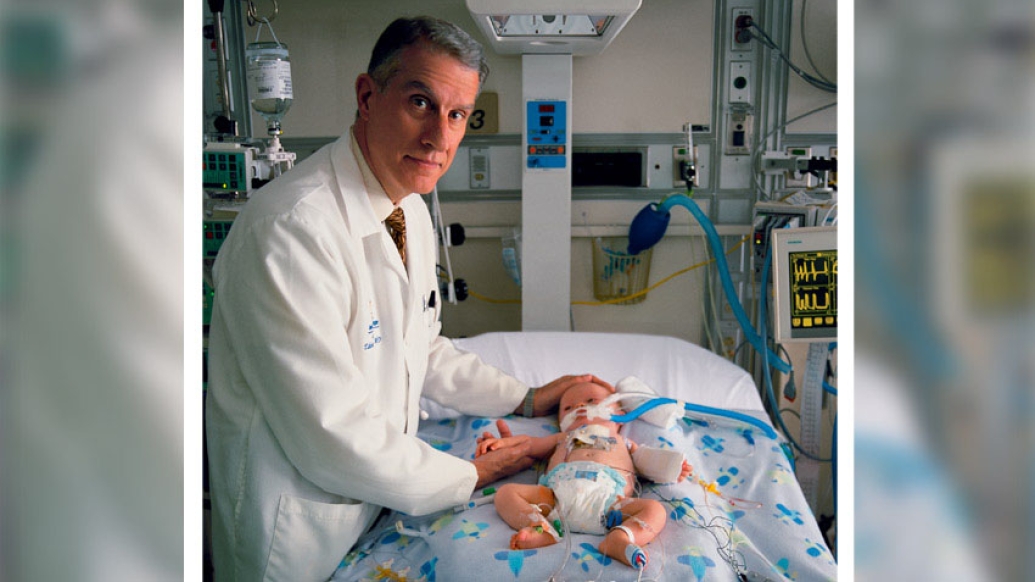
Very few will witness as drastic of advancements in their line of work within their lifetime as pediatric heart surgeon Edward L. Bove, M.D., has in the treatment of hypoplastic left heart syndrome. The complex congenital heart defect, sometimes referred to as a "half a heart," is a condition that is so severe that babies must undergo surgery within days of being born in order to survive.
Normal hearts have two ventricles – a left ventricle to pump blood out to your body and a right ventricle to pump blood to your lungs. In HLHS, instead of having two pumps, you have one.
Nearly 40 years ago, children born with HLHS didn't have operative solutions available to treat them, and thus, no chance of survival. Fast forward to today and C.S. Mott Children's Hospital, a high-volume pediatric heart center, proudly reports a 97% survival rate.
Since the 1980s, surgical treatment for HLHS evolved from nonexistent to a three-stage operation process: the Norwood operation, the hemi-Fontan operation and the Fontan operation.
But the road to get there was anything but easy.
The Norwood operation, invented by Bill Norwood, M.D., was first performed in 1983. At the time, death was extremely high. Even in the 90s, a paper was published stating the survivorship of Norwood operations across the United States was only about 40%, leaving many to believe it shouldn't be performed.
However, in the 1990s, Bove began seeing survival rates that were twice that – around 80%. His work in-particular was essential to the success of perfecting the second stage of the operation process called the hemi-Fontan.
Bove recently retired and transitioned to Professor Emeritus status after 40 years of caring for children with congenital heart disease.
Fortunately, though, his work lives on.
Over the course of his career, Bove trained around 40 congenital heart surgeons – 10 of whom now lead congenital heart programs on their own in the U.S. (including the Congenital Heart Center at University of Michigan Health C.S. Mott Children's Hospital) and throughout the world.
Bove recently was interviewed for a webinar where he discussed the evolution of heart care and what he sees for the future. Read below for highlights from the conversation, or watch the segment in its entirety.
You're renowned for your work advancing treatments for single ventricle heart defects – specifically hypoplastic left heart syndrome – but less people know you for arterial switch operations. At the time, doctors were criticized for arterial switch operations because it was a higher-risk operation [than the atrial switch]. Can you tell us what it's like to swim upstream?
Bove: It comes back to when I was in London. On Wednesdays, the two attending surgeons would go to a place called the Harley Street Clinic to operate and I would go over to assist. Most often, even when their case was done, I would stick around because a very renowned, phenomenal surgeon by the name of Sir Magdi Yacoub would also be operating over there. He had started taking newborns with transposition [of the great arteries] and banding the pulmonary artery to keep the left ventricle prepared and then doing [arterial] switches. He was getting tremendous criticism for that because the early mortality for the atrial switch operation was low but the late outcomes were not as good for many of these patients who would come back with problems.
When I came back to New York, our cardiologists there were also seeing patients come back with problems such as right ventricular failure and tricuspid regurgitation. I remember we sat down and determined we should start doing the [arterial] switch. The team of cardiologists and nurses were on board and said, "yes, let's do that. This is the way to go."
I still remember my very first switch – a baby at the time and now a young woman. For many, many years she would write me a letter every year. She's now probably in her late 30s and has kids of her own. The results right off the bat were good – we didn't have high mortality or any major problems – but it was pretty obvious from the get-go that was the way to go.
Without the collaboration and support of the cardiology team, we never would have gotten there.
Talk about your journey in operating on hypoplastic left heart syndrome.
Bove: I started in the mid-80s and, once again, in collaboration with pediatric cardiology. In that era, the only option was to let these babies die and there were too many of them that were, otherwise, beautiful, healthy-looking babies. It was too sad to deal with.
I started in Syracuse and, sadly, the first six babies I operated on never got off the OR table. The way we were doing it was wrong and we didn't really know. We were trying to learn.
You don't operate on a baby. You operate on a family. I can't ever tell you what that feeling is like.Edward L. Bove, M.D.
Then lucky No. 7 came along. The baby got off the OR table and there was no ICU bed ready because the ICU nurses figured why bother. Sure enough, we eventually got the bed! The baby was fairly sick and the first thing he taught me was that too big of a shunt was the worst thing in the world. We originally thought the bigger the shunt, the pinker the baby, but it was quite the opposite.
This baby survived and I ended up transitioning to Michigan. Around 8 to 10 months old, lucky No. 7 came up to Ann Arbor for the second stage of surgery. We didn't know what to do at first because we didn't have any previous survivors get that far. So, we did a Fontan operation, the old-style Fontan, which was absolutely not the way to do it, but we didn't know.
The child eventually died after about a month, and I was ready to quit. That was it for me. But I got a letter from that child's mom and dad thanking me for the nearly one year they had with their child and told me to keep trying, to not give up. It was very emotional, and I never forgot that.
I finally came around and thought, "okay, we've got to keep trying."
As a team, we started working on more cases but, at the time, there weren't a lot of referrals because people didn't think it was the way to go. Slowly, we started getting better results. Then we had to learn what to do when these patients came back six to eight months after the Norwood operation.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcasts or anywhere you listen to podcasts.
I had started using smaller shunts, but the babies were turning blue as they got older. Do we do another shunt? Do we do another operation rather than repeating the history? We struggled with that for a while until we finally stumbled upon the so-called hemi-Fontan – or bidirectional Glenn operation – what now is the second stage of the three-stage operation process.
It was in the early to mid-90s that we wrote a paper where we had over 80% survival for stage one which was incredible at the time, given the fact that no one was getting more than half of that. All of a sudden, referrals picked up. One year we did 66 Norwood operations. It was a dramatic difference, but it was step-by-step. I don't think there were any great come-to-Jesus moments, except lucky No. 7 who taught me about the shunt. It just changed the outcome completely.
Now I'm getting graduation letters and wedding invitations from young adults with this condition who are now living well into their 30s. It's overwhelming when you think about it. [University of] Michigan [Health] is now up to well over a thousand Norwood operations and even more Fontan operations, the second largest volume in the world.
Can you speak more to the hemi-Fontan operation and how it came to be the second stage of the three-part operation series? Did you ever consider changing it to a bidirectional Glenn? Have you tried to convert your previous trainees at other institutions to give it a try?
Bove: I started with the Glenn. In fact, one of my long-term survivors had a classic Glenn at the second stage because we couldn't figure out what to do. One of the problems I found with the Glenn was that, although it's technically easier to do, it doesn't necessarily fix the branch PAs (pulmonary arteries) which very often need to be enlarged.
I didn't start the hemi-Fontan [operation], but I remember reading about it and thinking that it was really a good idea for a number of reasons. It allows you to fix the branch PAs making them nice and big, getting rid of the potential risk associated with it, then to be able to complete the Fontan [operation] in a much easier fashion because you didn't have to dissect all that out again.
Since I've done that, we've done a number of computer flow studies looking at how the hemi-Fontan, and then subsequent lateral tunnel Fontan, distribute blood flow to each lung and minimize energy loss. Because you want to be as close to 50/50 as you can get. What our computer studies showed was that the hemi-Fontan and the lateral tunnel were by far better than a Glenn and an extra-cardiac (heart) conduit.
I've never changed from that because I've seen way too many – now adults – with lateral tunnel Fontans and their imaging looks great. It looks like it's grown with them, and they don't have any – or very minimal – foreign material.
A number of programs have switched to [the Glenn] because they think the hemi-Fontan is too complicated and they don't like to do it. I don't blame them but after having done literally thousands, to me, it's routine – as it is to our other Mott heart surgeons now – and we like it. It's hard to think to do it a different way when the long-term results have been outstanding.
What is the most important question about congenital heart surgery that you have yet to find the answer to? In other words, what's the next big thing?
Bove: We transitioned so much from just trying to get to survivorship into making sure now that we have a quality result and that means neurodevelopmentally and in many other ways as well. That's probably where the next years will bring us.
As we refine our techniques, we get better and better to make the methods we use for bypass and other surgical repairs lead our patients to be healthy in every way – by that, I mean mentally as well as physically.
MORE FROM THE LAB: Subscribe to our weekly newsletter
We're also going to be looking at the era – I hope, anyway – of stem cells. I think that's potentially the next biggest addition and transition we may have. Where we can grow valves, grow blood vessels, maybe even grow heart chambers, grow conduction (pacemaker of the heart) tissue – there's almost no limit as you think about what potentially that could bring us. It's a difficult thing and it's not right around the corner, but I think it's going to be there.
I think probably the third big thing is going to be devices. We've already gotten to the point where we have these devices that are much smaller, much more patient friendly and I think that's only going to get better. We will literally be able to support hearts with these miniature devices that will allow our patients to lead very good, useful, normal lives. That's a reality that's happening now and I think it's only going to get better.
How does it feel to know you have saved so many lives? There is no way, as a parent, to express our gratitude.
Bove: Well, thank you. There's no way I could ever tell you the respect and admiration I have for the parents. The parents are the heroes in all of this. I never took it lightly that parents were putting their baby in my arms to do something that is potentially lethal. I never took that lightly. The trust that they had is overwhelming – it still is.
A lot of people have asked what the greatest enjoyment is I've had, and I think the greatest enjoyment I've had – and it never got boring – was coming up and talking to the parents after surgery to let them know that everything was fine and their child was going to do well. Seeing the look on parents' faces and the relief and joy they had – you can't beat that. You don't operate on a baby. You operate on a family. I can't ever tell you what that feeling is like. It is truly unbelievable.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





