A laboratory-created microscopic network of fibers helped researchers understand how white blood cells capture and even kill bacteria, offering insight into the effectiveness of antibiotics in the future.
2:55 PM
Author |

Experiencing a bacterial infection? You're generally prescribed antibiotics by your doctor.
But how exactly do those antibiotics and your white blood cells work in tandem to improve your infection?
"The human body's first line of defense against bacteria are certain white blood cells called neutrophils," says J. Scott VanEpps, M.D., Ph.D., assistant professor of emergency medicine at Michigan Medicine. "One of their weapons are neutrophil extracellular traps, also called NETs."
The traps are microscopic networks of fibers made primarily of DNA that are produced by the neutrophils to capture bacteria. But how exactly they work, VanEpps notes, is still unclear.
The knowledge gained in this study could be helpful in the future in designing new and better antibiotics that mimic the body's natural defense mechanisms, as well as potentially change how we dose antibiotics …- J. Scott VanEpps, M.D., Ph.D.
"The exact function and mechanism of NETs remains a bit of a mystery likely because they have different functions for different situations," he says. "And it's very hard to isolate these NETs in the laboratory and study them in detail."
VanEpps is a co-senior author of a new study, published in Advanced Materials, that investigated if there was a way to successfully create NETs in the laboratory to better understand how NETs can capture bacteria.
"We were hoping to provide a bottom-up engineering approach to better understand how the immune system fights bacteria, specifically the immune system's weapon: NET," says VanEpps, associate director at the Michigan Center for Integrative Research in Critical Care.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
Recreating and studying networks
VanEpps explains that he and the team found their first surprising finding during the recreation of the NETs.
"Although there are literally hundreds of different ingredients in natural NETs, we were able to recreate a lot of their structure and function with just two ingredients and determined the optimal ratio of those ingredients," he says. "They look and function very similar to NETs produced by those neutrophil white blood cells and the synthesis method is much simpler than isolating them from neutrophils."
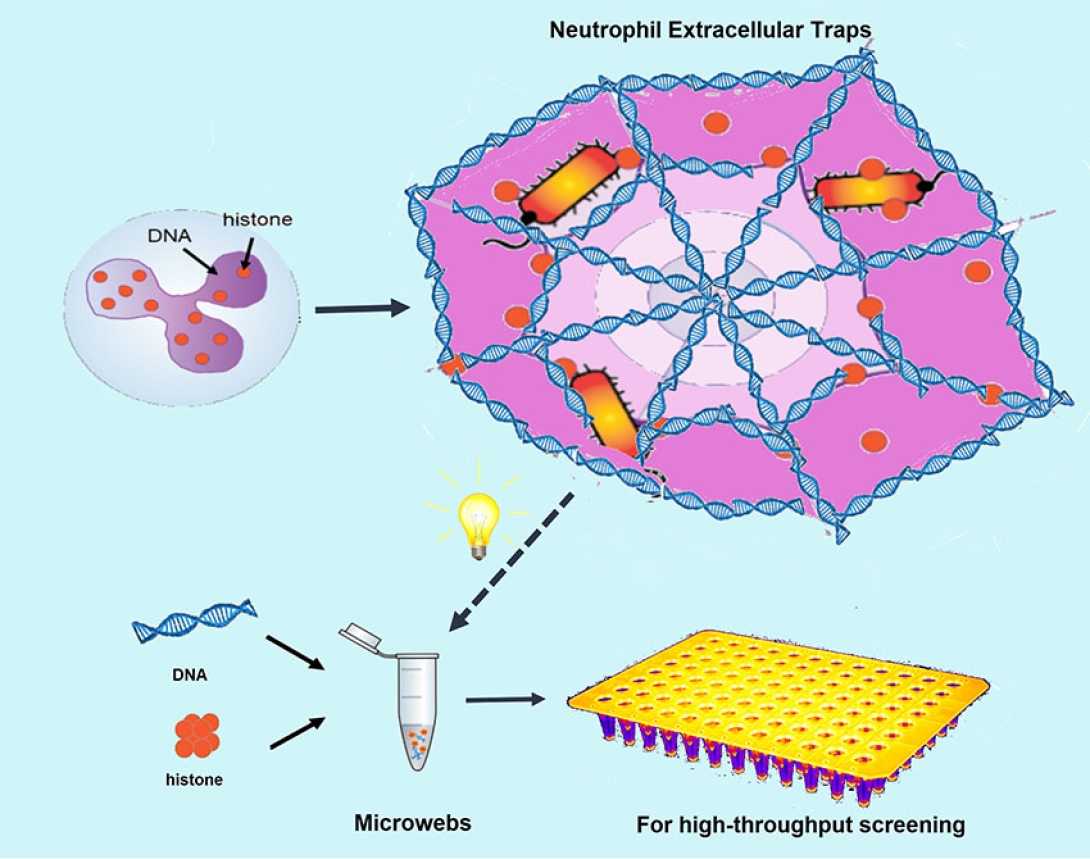
After producing the microwebs, the research team studied them more closely to provide a more detailed understanding of how NETs can capture, and the second surprising finding of the study, even kill bacteria.
"We studied how our microwebs capture E. coli and found they could also kill it," VanEpps says. "This led to us examining how microwebs might play a role with antibiotics.
"Importantly, we found that the dose of antibiotic required to kill E. coli (including a colistin resistant strain of E. coli) was less when our microwebs were present."
MORE FROM THE LAB: Subscribe to our weekly newsletter
VanEpps' co-senior author, Shuichi Takayama, Ph.D., a professor at Georgia Tech, says the findings are an example of teamwork.
"This research was an outstanding team effort," Takayama says. "Microbiology from the VanEpps lab, NET-like materials contributions from the Moon lab, NET expertise from the Knight lab, colistin resistance expertise from the Weiss lab and Yang Song, Ph.D., leading the effort, made this all come together."
Future research
VanEpps notes this study can be a jumping off point for future research.
"Now that we have a platform, we can synthesize microwebs with different NET components to more precisely describe how the immune system uses NETs in different situations," he says.
This understanding of the body's natural killing of bacteria could also help in developing new treatments for infections.
"The knowledge gained in this study could be helpful in the future in designing new and better antibiotics that mimic the body's natural defense mechanisms, as well as potentially change how we dose antibiotics given the potential synergy between the immune system and certain antibiotics," VanEpps says.
"That's critical as we have not developed a new class of antibiotics in over 30 years and resistance continues to increase."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!