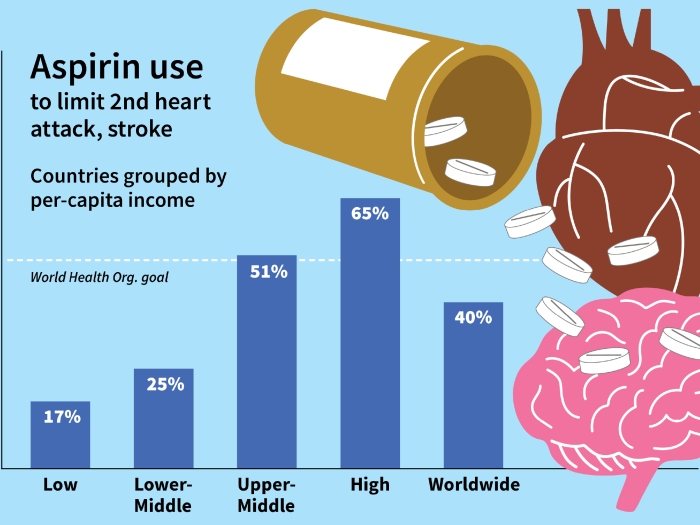
Forty percent of people who develop venous thromboembolism don’t know what caused it. New research in mice further explores inflammation’s role.
4:43 PM
Author |
It's the third deadliest cardiovascular diagnosis, but doctors are still often stumped to explain why 40% of patients experience unprovoked venous thromboembolism (VTE). And after a patient has dealt with these dangerous blood clots once, a second clot becomes much more likely.
Recent research from Michigan Medicine scientists may help solve the mystery of how to detect and deal with higher-than-usual clot risk in patients' veins. The study, done in mice and published in the Journal of Clinical Investigation, focuses on clots' relationship to the body's defense and repair system, which causes inflammation.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
"We don't yet understand the molecular triggers which drive the development of life-threatening clots in deep veins," said Yogen Kanthi, M.D., the study's senior author and a vascular cardiologist at U-M's Frankel Cardiovascular Center. "Our work aimed to identify and block a previously unrecognized pathway linking inflammation and thrombosis."
Kanthi, also an assistant professor of internal medicine at Michigan Medicine, says some combination of coagulation and inflammation triggers VTE. But current treatments come up short, he says, because they only focus on one side of the equation: anticoagulation. After VTE, patients are often prescribed blood thinners for life.
Kanthi's lab is instead investigating inflammation's role in the development of deep vein thrombosis. His team's new study found an enzyme called CD39 diffused circulating "danger" signals and inflammatory cytokines in blood during thrombosis.
FDA-approved drugs already exist for other conditions that are affected by the same pathway, and in particular, the paradigmatic inflammatory cytokine molecule called interleukin-1 beta. In fact, when the researchers inhibited those interleukin-1 signals in their study, they reduced the number and size of venous blood clots the animals formed, Kanthi said.
"Here, we focused on potential therapeutics at the intersection of inflammation and thrombosis," Kanthi said. "We found that blocking interleukin 1 signals was a powerful means to stop dangerous clotting."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Treatment guidelines recommend lifelong blood thinners for people who have had an unprovoked clot, but anticoagulation carries other risks, like bleeding, and can be burdensome for patients, Kanthi says.
Some of the people at highest risk have underlying disorders that tend to cause inflammation, including autoimmune disorders like lupus or Crohn's disease.
"We continue to uncover more about the risk factors in VTE, including the connection between coagulation and inflammation, which we believe will one day lead to new, better therapeutics for patients," says Vinita Yadav, Ph.D., a research lab specialist at the Frankel CVC. Yadav is co-first author with Liguo Chi, M.D., Ph.D., a former lab surgeon at the Frankel CVC.
Earlier this year, Kanthi and colleagues published a paper in Arteriosclerosis, Thrombosis, and Vascular Biology that identified CD39 as important to the venous thromboinflammatory response.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!