New research finds the protein PDX1 is critical for cancer growth, but blocking it may lead to more aggressive tumors.
7:00 AM
Author |
A protein thought to fuel pancreatic cancer development plays a much more complicated role than previously believed, a new study finds.
MORE FROM THE LAB: Subscribe to our weekly newsletter
PDX1, a transcription factor critical for pancreatic development, has distinct roles at different stages of pancreatic cancer: keeping cancer at bay in normal cells, then eventually contributing to the cancer's growth once a tumor forms and also preventing the tumor from becoming more aggressive.
It's a complexity that seems to be typical of this challenging disease, which is the No. 3 cancer killer.
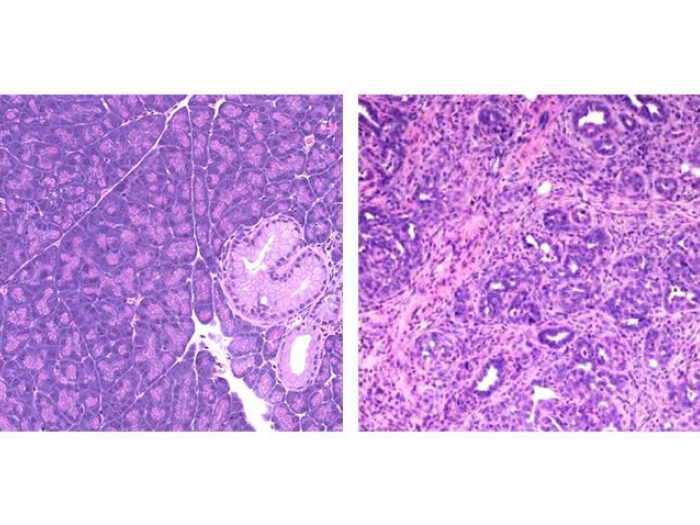
Researchers from Michigan Medicine and the University of California San Francisco used mouse models to look at normal pancreas cells, a type of precancerous pancreas lesion called PanIN and pancreatic cancer cells. In the normal cells, PDX1 maintains the cells' identity as pancreas cells and epithelial cells. The protein is required for a wound-healing process to regenerate the damaged organ and maintain normal cell function.
But once cells become malignant, PDX1 takes on a new role and contributes to the cancer's growth. This activity has made it an attractive target for developing potential pancreatic cancer treatments: Block PDX1, and the cancer won't grow.
Inhibiting PDX1 can be temporarily effective. But we need to be prepared for the mechanism of resistance and for the likelihood of making the cancer more aggressive.Howard Crawford, Ph.D.
The new study, published in Genes & Development, finds a significant twist.
When researchers looked at subtypes of pancreatic cancer, they found the lowest levels of PDX1 were in the most aggressive cancers. The patients whose tumors had no PDX1 had the worst outcomes.
"PDX1 has been reported as a target to treat cancer. The reality is that might not be the best idea," says study author Howard Crawford, Ph.D., professor of molecular and integrative physiology and of internal medicine at the University of Michigan Medical School.
SEE ALSO: Giving Pancreatic Cancer Patients More Shots on Goal
Although the protein functions to promote the cancer's growth, Crawford explains, ultimately turning off PDX1 makes the cancer more aggressive.
"We showed the loss of PDX1 is actually promoting the aggressiveness. Losing PDX1 means the cells lose their identity," Crawford says.
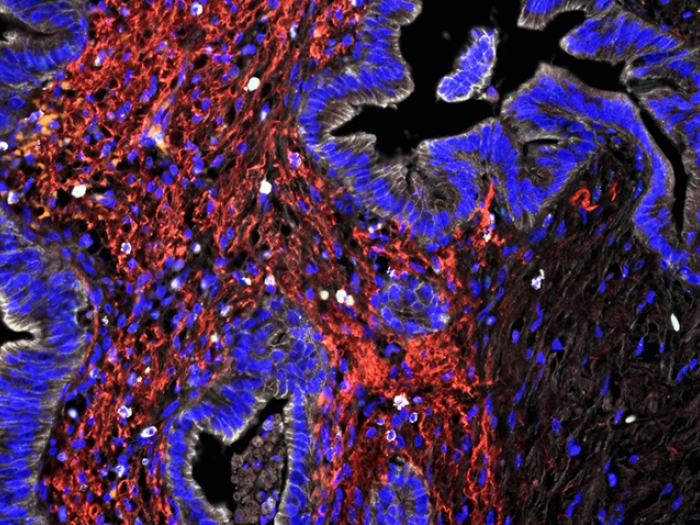
The researchers found that this loss of identity allows the relatively well-behaved epithelial cells to transition to bad-acting mesenchymal cells, which are more likely to move throughout the body — the hallmark of metastatic cancer, which is the primary cause of cancer recurrence and patient death.
When PDX1 is lost, the researchers found, it selects for cancer cells that express MYC, which is known to be involved in cancer growth and metastasis.
"We need to be cautious about targeting PDX1. If we do target it, the cancer will escape treatment by upregulating MYC, so we need to be prepared to target that, too," Crawford says. Inhibitors are being developed that have shown some effect on cancers expressing MYC.
Crawford compares PDX1 to the estrogen receptor in breast cancer and the androgen receptor in prostate cancer. Both define cell identity and are legitimate targets for treatment. But in both cases, tumors can become resistant to treatments — leading to the most challenging and aggressive types of those cancers.
"Inhibiting PDX1 can be temporarily effective. But we need to be prepared for the mechanism of resistance and for the likelihood of making the cancer more aggressive," Crawford says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!