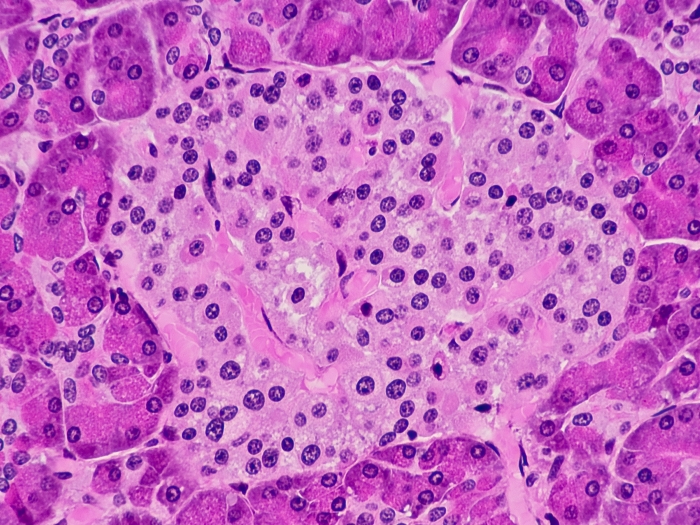
Viewing the amount of insulin in a living pancreas had never been done before. Now a U-M researcher has found a noninvasive way to shed light on pancreatic insulin.
8:00 AM
Author |
Scientists and doctors have long wanted to know how much insulin a person has but haven't been able to know the exact amount without physically removing the pancreas from a deceased patient for review.
But a new study in the journal Diabetes details how a group of researchers was finally able to visualize stored insulin in the pancreas of a living creature — in this case, a mouse.
"In the past, there hasn't been technology that would afford us this same opportunity," says Peter Arvan, M.D., Ph.D., division chief of Metabolism, Endocrinology & Diabetes at the University of Michigan Health System and a co-author of the study.
To gain that once-elusive glimpse, Arvan and his fellow researchers genetically engineered a mouse that, like humans, makes a protein, proinsulin, used to produce insulin.
By engineering the proinsulin as a fluorescent protein, it emitted a fluorescent light when researchers shined a light of certain wavelength on the mouse's pancreas. In other words, the pancreatic islets — tiny clusters of cells in the pancreas that include the insulin-making beta cells — bounced a special wavelength of light back. The strength of the fluorescent signal indicated how much proinsulin and insulin were present.
It has been a holy grail to try to look inside a living person's pancreas and see how much insulin that person has stored away. This study is an important and exciting first step.
Researchers were able to see, in real time, when the mouse was releasing its insulin by giving the animal sugar water (glucose). After glucose entered the stomach and blood sugar began to rise, insulin was released in response, and fluorescence was released from some of the islets.
When isolated pancreatic beta cells were stimulated the same way, individual fluorescent flashes indicating secretion of small packets of insulin from the cells could be observed. When the beta cells were not stimulated, insulin release was low and no flashes were seen. These findings indicated the amount of fluorescence lost from beta cells was proportional to the amount of insulin released.
Varying levels of response
Such illuminations led the researchers to learn something else: Not all islets are created equal.
"We could see responses in specific pancreatic islets that appeared especially good at releasing insulin into the bloodstream," Arvan says. "Amazingly, only a small fraction of the pancreatic islets showed a major response to glucose, while the rest of the islets appeared to remain mostly inactive."
This surprising result, according to Arvan, implies that only a portion of the body's islets represent the first line of defense against high blood sugar — an observation that before this study had never been made.
"Perhaps only after we have lost our first-responder islets do we recruit backup islets to provide insulin," Arvan says.
The activating of those backup islets has potential future clinical implications that could help patients with diabetes, Arvan adds. For now, the initial victory of measuring the once-unmeasurable has Arvan and his team hopeful for new developments rooted in their findings.
"It has been a holy grail to try to look inside a living person's pancreas and see how much insulin that person has stored away," Arvan says. "This study is an important and exciting first step."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!