Vessel-sparing radiation combined with a better understanding of prostate anatomy can help preserve patients’ sexual function, a new paper says.
5:50 PM
Author |
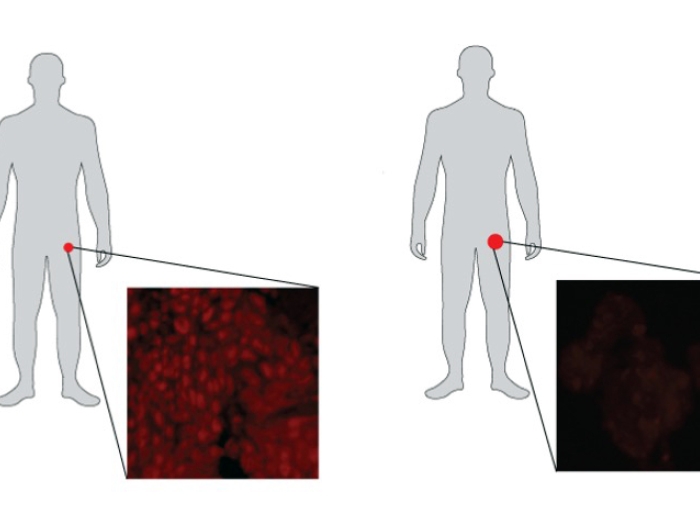
The prostate is a tiny organ surrounded by critical structures.
When radiation treatments for prostate cancer deliver doses to any of these structures, it sometimes leads to problems such as erectile dysfunction and bladder or rectal irritation.
"We always have to keep cure as our first priority, but quality of life is a major secondary concern for men with prostate cancer," says Patrick W. McLaughlin, M.D., professor of radiation oncology at the University of Michigan Medical School.
"In the past, cure came at a steep price in lost quality of life, but with modern refinements it is increasingly possible to meet the new standard of successful prostate cancer treatment: cure with quality of life," he says.
McLaughlin is the senior author of a paper published in Lancet Oncology that examines how MRI and a clear understanding of the functional anatomy (and its variations among patients) can allow radiation oncologists to plan a course of treatment that spares these critical structures.
The team started by defining the critical functions and structures that run through or near the prostate. These include the nerves, vessels and sphincters that control bladder function, erectile function and rectal function.
"The benefit of the functional anatomy approach goes well beyond improving sexual function. It has improved urinary and rectal function as well," McLaughlin says.
Both radiation oncologists and surgeons are conducting ongoing research to improve their understanding of the functional anatomy. This is critical for both disciplines as they work to eliminate cancer while preserving function.
"We argue that current rates of side effects and changes after treatment are not fixed, and that further potential improvements in function preservation are possible and likely by pursuing this vessel-sparing approach," says co-author Jae Lee, M.D., Ph.D., a radiation oncology resident.
In the past, cure came at a steep price in lost quality of life, but with modern refinements it is increasingly possible to meet the new standard of successful prostate cancer treatment: cure with quality of life.Patrick W. McLaughlin, M.D.
MRI as guide
The study authors also found that MRI was a critical tool for accurately outlining the prostate anatomy and planning radiation therapy. They could easily and precisely see the borders of the prostate on an MRI. CT images are much less clear, and it's common to overestimate the area that needs to be treated. With a clear outline of the prostate and other structures on an MRI, radiation oncologists can precisely target treatment to the prostate while avoiding critical erectile tissues. The technique is called vessel-sparing radiation.
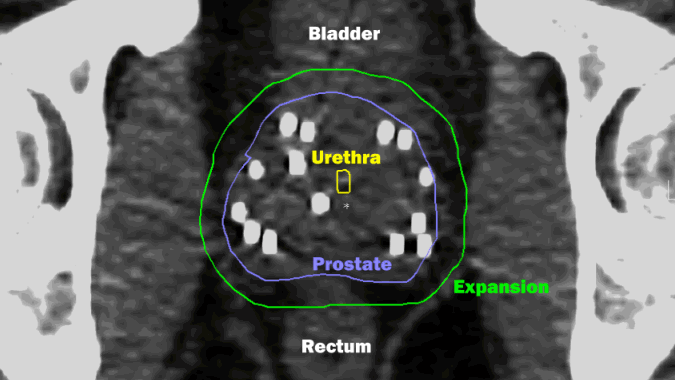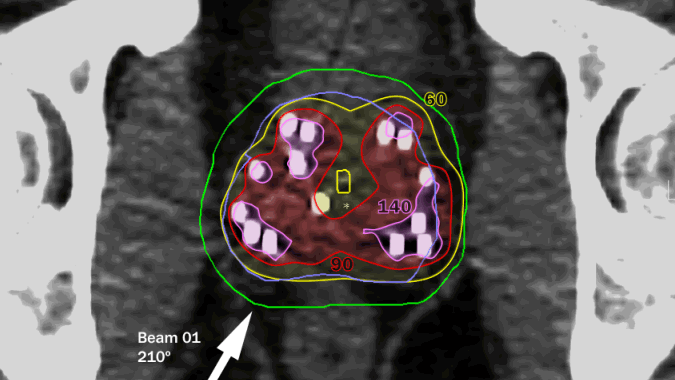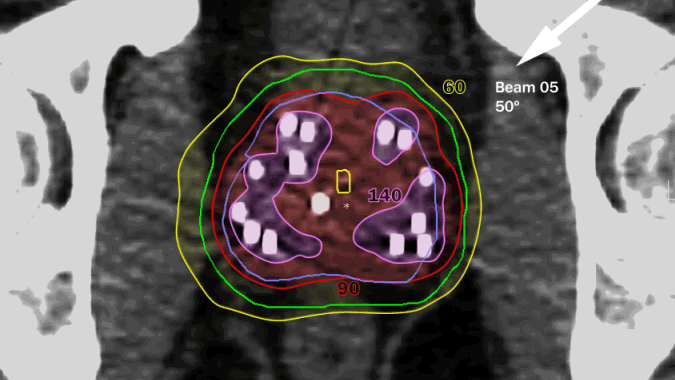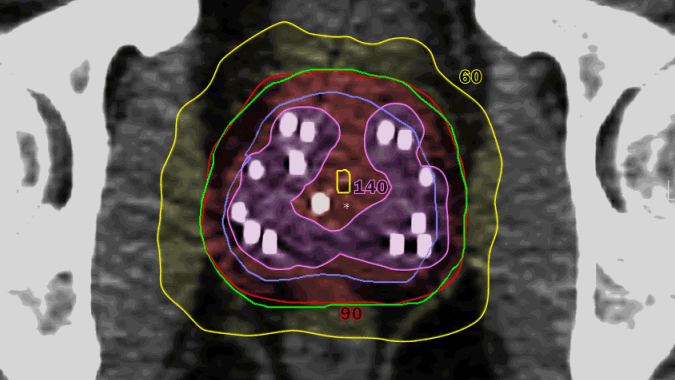
Radiation dose is delivered by beams directed from many angles combined with implanted seeds (white spots). By integrating the two types of radiation, the highest dose is delivered only within the tumor. The external beams correct any irregularity from the seeds. Thanks to MRI planning, very little dose goes to critical adjacent structures.
Of 49 patients treated with a combination of seeds plus external beam radiation with at least five years of follow-up, 92 percent reported they were still able to be sexually active.
"We found no difference in quality of life for men given aggressive treatment. If you define the functional structures and limit dose to them, you can achieve cure and excellent quality of life," says co-author Daniel E. Spratt, M.D., chief of the genitourinary radiation oncology program at the University of Michigan.
Vessel-sparing radiation requires that physicians train in MRI anatomy to recognize and identify key structures. McLaughlin has previously developed a tool that is available free online called Prostadoodle. It includes a section on defining the erectile vessels.
In addition, MRI could be helpful in guiding patients to the best treatment option based on their unique anatomy.
Is the tumor outside of the prostate gland? That would suggest the need for radiation therapy after surgery, if surgery is chosen as the primary treatment. Does the patient have a short urinary sphincter? Although rare, these patients have a higher risk of incontinence after surgery.
"For patients who appear to have slow-growing, non-aggressive cancers, MRI can confirm there is no aggressive cancer present. For such patients, surveillance is an excellent choice," McLaughlin says. "By avoiding treatment altogether when appropriate, all the side effects and quality-of-life impact from treatment is avoided.
"On the other end of the spectrum, MRI may actually reveal more serious cancers not sampled by the biopsy. This can shift treatment to a more aggressive approach necessary to cure such cancers."
McLaughlin sees patients at the Assarian Cancer Center at Providence Park in Novi and Providence Cancer Center in Southfield, Michigan, which is part of the University of Michigan's Radiation Oncology Network. All the research was completed at the Providence affiliate.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!