A new study in mice suggests that low-fiber diets prompt a gut bacteria response that may leave the colon vulnerable to infection.
12:00 PM
Author |
It sounds like the plot of a 1950s science fiction movie: normal, helpful bacteria that begin to eat their host from within because they don't get what they want.
MORE FROM THE LAB: Subscribe to our weekly newsletter
New research shows that's exactly what happens when microbes inside the digestive system lack the natural fiber they rely on for food.
Starved, they begin to munch on the natural mucus that lines the gut, eroding it to the point where dangerous invading bacteria can infect the colon wall.
In a new paper in Cell, an international research team shows the impact of fiber deprivation on the guts of specially raised mice.
The mice were born and raised with no gut microbes of their own, then received a transplant of 14 bacteria that normally grow in the human gut. Scientists know the full genetic signature of each one, making it possible to track their activity over time.
The findings have implications for understanding not only fiber's role in a normal diet, but also its potential to counter the effects of digestive tract disorders.
"The lesson we're learning from studying the interaction of fiber, gut microbes and the intestinal barrier system is that if you don't feed them, they can eat you," says Eric Martens, Ph.D., an associate professor of microbiology at the University of Michigan Medical School who led the research along with his former postdoctoral fellow, Mahesh Desai, Ph.D., now a principal investigator at the Luxembourg Institute of Health.
This work ... amplifies everything that doctors and nutritionists have been telling us for decades: Eat a lot of fiber from diverse natural sources.Eric Martens, Ph.D.
Comparing fiber content
Using U-M's special gnotobiotic, or germ-free, mouse facility and advanced genetic techniques to determine which bacteria were present and active under different conditions, the researchers studied the impact of diets with different fiber content — and those with no fiber.
They also infected some of the mice with a bacterial strain that does to mice what certain strains of Escherichia coli can do to humans: cause gut infections that lead to irritation, inflammation, diarrhea and more.
SEE ALSO: Gut Bacteria Leads to Obesity? Not So Fast
The result: In mice that received a diet that was about 15 percent fiber from minimally processed grains and plants, the mucus layer stayed thick and the infection didn't take full hold. But when the researchers substituted a diet with no fiber, even for just a few days, some of the microbes in the gut began to erode the mucus.
Investigators also tried a diet that was rich in prebiotic fiber — purified forms of soluble fiber similar to what some processed foods and supplements contain. This diet resulted in a similar erosion of the mucus layer as observed in no-fiber conditions.
The researchers also saw that the bacterial mix changed depending on what the mice were fed, even day by day. Some species of bacteria in the transplanted microbiome were more common — meaning they reproduced more — in low-fiber conditions, while others reproduced more in high-fiber conditions.
The four bacteria strains that flourished most in low-fiber and no-fiber conditions were the only ones that make enzymes capable of breaking down the long molecules called glycoproteins that make up the mucus layer.
In addition to looking at the bacteria based on genetic information, the researchers could see which fiber-digesting enzymes the bacteria were making. They detected more than 1,600 enzymes capable of degrading carbohydrates — similar to the complexity in the normal human gut.
Just like the mix of bacteria, the mix of enzymes changed depending on what the mice were fed, with even occasional fiber deprivation leading to more production of mucus-degrading enzymes.
Images of the mucus layer, and the "goblet" cells of the colon wall that produce the mucus constantly, showed the layer was thinner the less fiber the mice received. While mucus is constantly being produced and degraded in a normal gut, the change in bacteria activity under the lowest-fiber conditions meant that the bacteria were eating the mucus faster than it was being produced — almost like an overzealous harvesting of trees outpacing the planting of new ones.
When the researchers infected the mice with Citrobacter rodentium — the E. coli-like bacteria — they observed that these dangerous bacteria flourished more in the guts of mice fed a fiber-free diet. Many of those mice began to show severe signs of illness and lost weight.
When the scientists looked at samples of the gut tissue from these mice, they saw a much thinner, or even patchy, mucus layer and inflammation across a wide area. Mice that received a fiber-rich diet before infection also had some inflammation, but across a much smaller area.
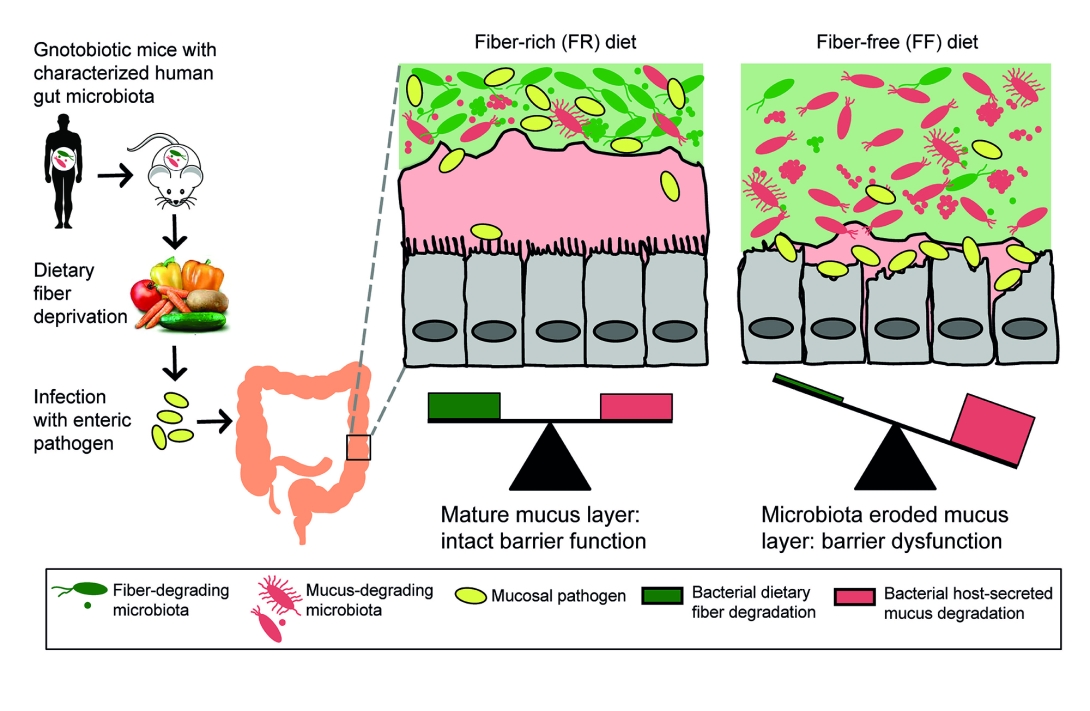
The take-home message
Going forward, Martens and Desai intend to look at the impact of prebiotic fiber mixes and of diets with more intermitted natural fiber content over a longer period. They also want to look for biomarkers that could tell them about the status of the mucus layer in human guts, such as the abundance of mucus-digesting bacteria strains, and the effect of low fiber on chronic disease such as inflammatory bowel disease.
"To make it simple, the 'holes' created by our microbiota while eroding the mucus serve as wide-open doors for pathogenic microorganisms to invade," explains Desai.
"While this work was in mice, the take-home message from this work for humans amplifies everything that doctors and nutritionists have been telling us for decades: Eat a lot of fiber from diverse natural sources," Martens says.
"Your diet directly influences your microbiota, and from there it may influence the status of your gut's mucus layer and tendency toward disease. But it's an open question of whether we can cure our cultural lack of fiber with something more purified and easy to ingest than a lot of broccoli."
Martens notes that in addition to the gnotobiotic facility, the research was possible because of the microbe DNA and RNA sequencing capability built up through the Medical School's Host Microbiome Initiative, as well as the computing capability to plow through the sequence data.
"Having all the resources here was the key to making this work, and the fact that it was all across the street from our lab allowed us to pin it all together," Martens says. He also notes the role of U-M colleagues led by Gabriel Nunez and Nobuhiko Kamada in providing the C. rodentium pathogen model and of French collaborators from the Aix-Marseille Université in studying the enzymes in the mouse gut. The work was funded by the National Institutes of Health, U-M and Luxembourg-based institutes.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





