A team led by U-M researchers discovered that a noninvasive imaging biomarker can identify small airway damage in COPD patients.
7:00 AM
Author |

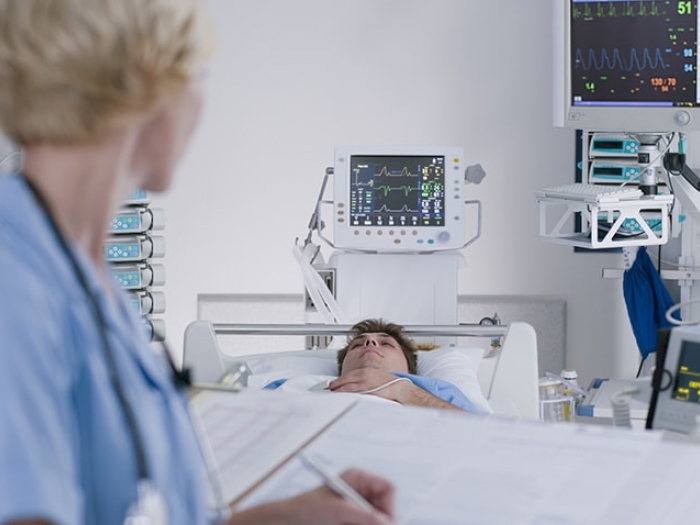
Chronic obstructive pulmonary disease (COPD), an inflammatory disease of the small airways in the lungs, affects 16 million Americans and is the fourth leading cause of death in the United States, according to the National Heart, Lung, and Blood Institute.
COPD causes breathing problems and blocks airflow in the body. Symptoms include shortness of breath, coughing, difficulty exercising and a history of asthma. It is diagnosed using spirometry, a breathing test that checks how well the lungs can inhale and exhale.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
Physicians would like to identify the disease in its earliest stages, when it is most treatable. But it is tricky to spot damage to the tiny airways, called bronchioles. The bronchioles are less than 2 millimeters in internal diameter — too small to be seen on CT imaging.
Noninvasive technique
But in a landmark study funded by the NHLBI, an international team of researchers led by Michigan Medicine discovered that a noninvasive technique that measures lung density during inhalation and exhalation — called parametric response mapping, or PRM — could identify the small airway damage common in early stages of COPD.
Brian Ross, Ph.D., a U-M professor of radiology and biological chemistry, and Craig Galban, Ph.D., a U-M associate professor of radiology, are credited with the PRM invention.
The team reported the findings in a recent issue of the American Journal of Respiratory and Critical Care Medicine.
"Now we have confidence in our ability to identify airway disease when imaging COPD patients," says senior author MeiLan Han, M.D., a U-M lung specialist and professor of internal medicine. "This is what we mean by bench-to-bedside medicine."
SEE ALSO: COPD Symptoms Common Among Smokers, Even When Undiagnosed
While these studies were performed in patients with severe disease, in another NHLBI-funded study, COPDGene, the PRM-defined small airway abnormalities have been detected on CT scans of patients with milder disease and help to predict patients who will lose lung function.
Han says there's more work ahead.
"We still need to validate the type of airway disease the PRM technique identifies in patients with milder disease," she says. "That type of lung tissue is more difficult to obtain, but we are working on techniques that would allow us to use smaller amounts of lung tissue to make such studies feasible."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Currently, there is no cure for COPD.
Lifestyle changes, such as quitting smoking, and treatment with bronchodilators and inhaled steroids can help expand airways and reduce inflammation. Surgery to remove damaged lung tissue and lung transplantation are options for some patients with severe disease.
SEE ALSO: Care for COPD: Could More Be Done?
Noninvasive measure
By helping to identify patients at risk for disease progression, PRM can serve as a noninvasive measure to aid clinical trials of new therapeutics, the researchers concluded.
"These results illustrate the importance of developing noninvasive techniques for improving diagnostic capabilities and advancing new therapies needed to tackle this devastating disease," says James Kiley, Ph.D., director of the Division of Lung Diseases at the NHLBI. "The refinement of this and similar approaches could also advance the study of COPD at its earliest stages of development."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!