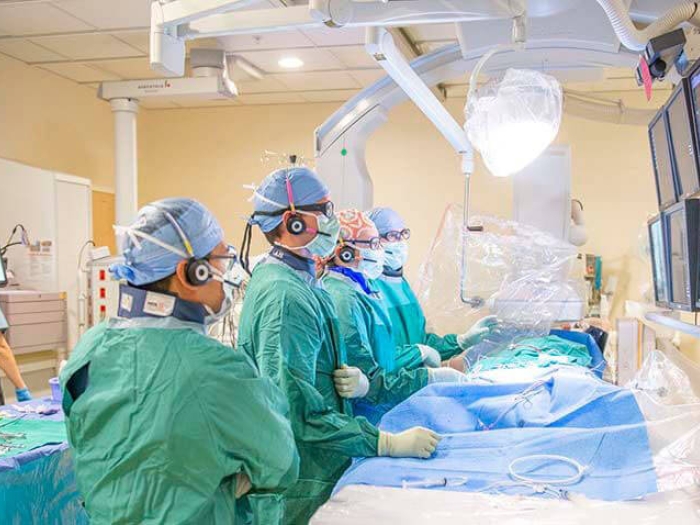
Researchers study stem cells’ potential to preserve heart function and delay heart transplants for children with complex congenital heart disease.
8:00 AM
Author |
Even after undergoing the most advanced treatments, some children with complex heart disease may still ultimately be left with one life-saving option: a new heart.
But doctors are hoping a novel clinical trial helps them learn more about whether there may be another alternative through stem cell therapy.
Researchers will look at whether stem cells, which have been shown to have regenerative effects in adult heart patients, could also preserve heart tissue in children to help them delay or possibly avoid heart transplants in the future.
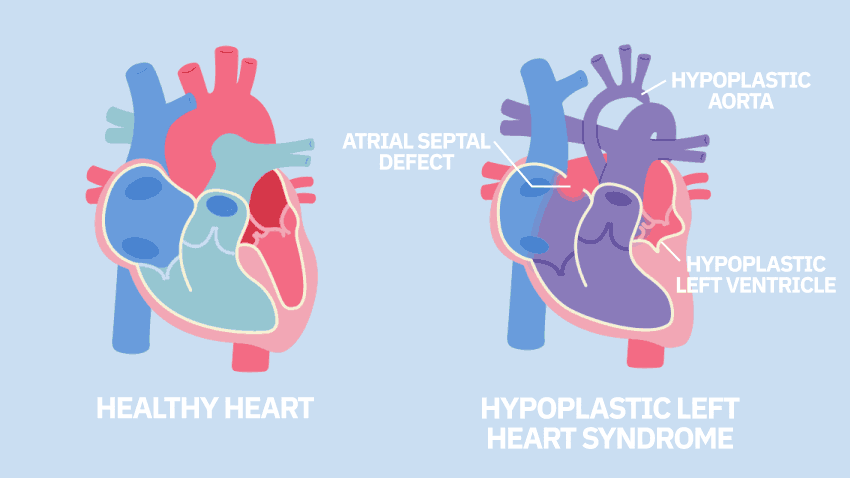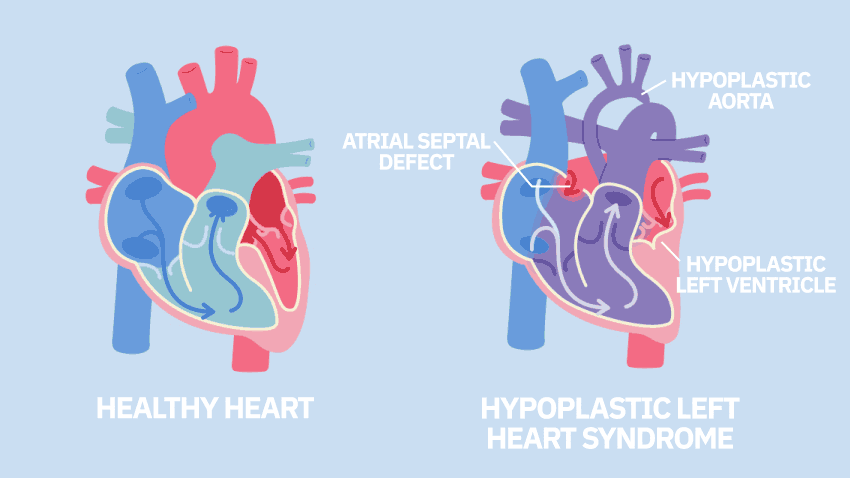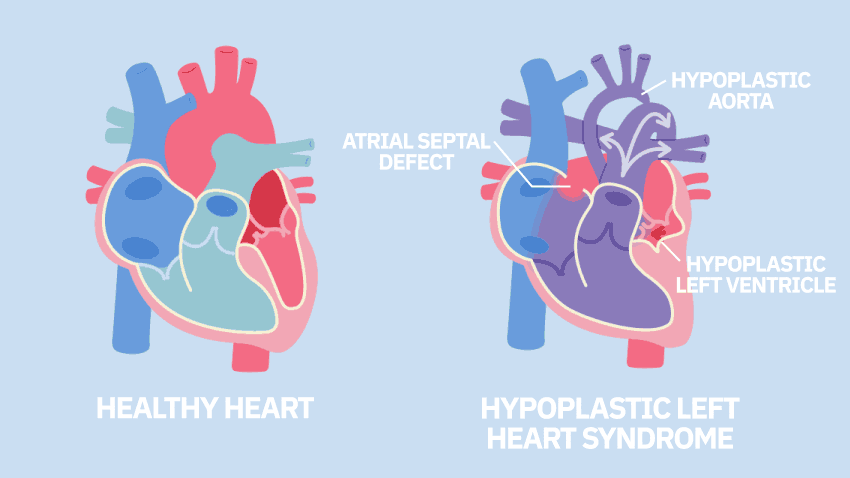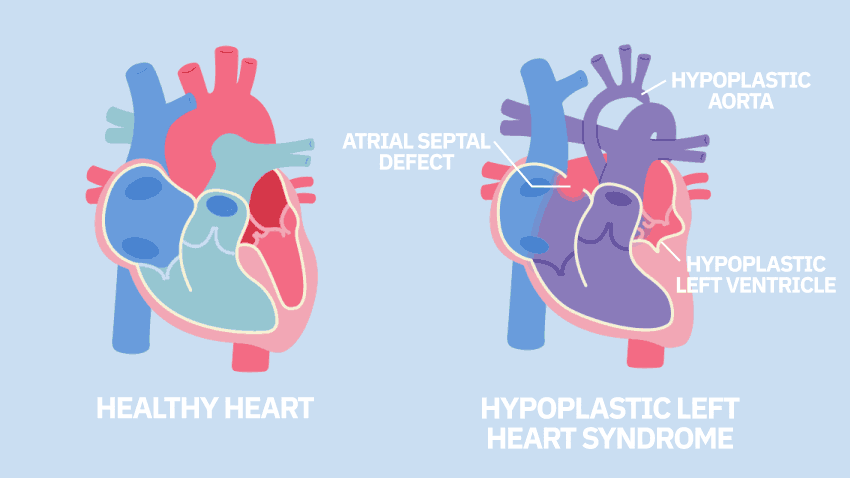
The University of Michigan Health C.S. Mott Children's Hospital, which has one of the largest congenital heart programs in the country, is among the first study sites to begin applying stem cell therapy to babies with single ventricle heart disease. The trial specifically includes children with hypoplastic left heart syndrome, a defect in which the heart's left ventricle is underdeveloped and can't effectively pump blood to the body.
"Despite significant strides in medical care and surgical techniques, long-term survival of children with failing single ventricles remains limited. For these families, the only viable medical therapy is a heart transplant," said Mott pediatric heart surgeon Richard Ohye, M.D., co-director of the hospital's congenital heart center.
"Research suggests that stem cell therapy may have the potential to strengthen and improve heart function in young patients who have no other treatment options. We hope this research provides more insight into the efficacy of regenerative medicine in children with these congenital heart conditions."
Hypoplastic left heart syndrome is one of the most complex forms of congenital heart disease, occurring in about 9% of children with a congenital heart defect.
Most babies with the condition undergo a series of three open heart surgeries during the first two years of life. The goal of these operations is to rebuild the heart so that the right side can be used to pump blood out to the body.
But over time, the right ventricle becomes overworked and stressed as it takes on the job of two ventricles. Heart function gradually declines, and there is currently no way to prevent or treat resulting heart failure.
While heart transplants can save these children's lives, the option is limited by donor availability, Ohye said, and those with hypoplastic left heart syndrome specifically are at higher risk of worse outcomes compared to other heart transplant recipients.
Mortality rates also remain as high as 25- 35% during the first year of life for babies with the condition.
How the stem cell treatment works
The multi-center randomized trial, known as the Autologous Cardiac Stem Cell Injection in Patients with Hypoplastic Left Heart Syndrome (CHILD), will compare outcomes between patients who receive the stem cell therapy and those who don't. When patients are enrolled, they will randomly be picked to be in either the stem cell or control group.
Research suggests that stem cell therapy may have the potential to strengthen and improve heart function in young patients who have no other treatment options.Richard Ohye, M.D.
Four clinical sites, including Mott, will be part of the CHILD trial, which is led by the University of Miami and Lurie Children's Hospital of Chicago.
Stem cells, which are believed to release healing proteins that may stimulate the heart to repair defective heart muscle, must be extracted from babies during their first open heart surgery as newborns.
The tissue will then be sent to an external lab for cardiac stem cell isolation and expansion and back to the trial site. During the second surgical repair four to six months later, Mott pediatric heart surgeons will inject the stem cells into infants' hearts.
Doctors hope that the stem cells will have a reparative effect and prevent deterioration of existing heart tissues and strengthen the working right ventricle while the baby is young and the heart is still developing.
Patients will be followed for at least a year with blood tests, echocardiograms and MRIs to reinforce safety and efficacy.
"These are patients who are at extremely high risk of eventually developing heart failure," said Ming-Sing Si, M.D., who was a pediatric heart surgeon at Mott for nine years and helped launch the trial at the hospital.
"Some may not need a new heart until they're adults, but many others end up on a heart transplant waiting list much earlier, possibly in their first 10-15 years of life.
"This complex type of congenital heart disease affects thousands of kids in the U.S. every year," he added. "The Mott congenital heart program is joining a select group of centers in the country that have a shared mission and commitment to seeking innovative treatments for these children."
The Mott congenital heart center sees among the highest caseloads of complex single ventricle heart cases in the country, with between 20 and 30 patients a year and almost 1,200 over the last few decades.
"As a national and international center specializing in congenital heart single ventricle disease, we take care of a high volume of children with very complex heart conditions," Ohye said.
"We remain dedicated to investigating new therapies that will help us improve care and outcomes for congenital heart patients with limited treatment options."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!