Tough conversations — and treatment decisions — are necessary after a complex diagnosis. A Michigan Medicine vascular surgeon designed a tool to help start them.
1:00 PM
Author |

After a complex diagnosis, it's crucial to consider a patient's values and desires when discussing treatment options. But those conversations can become long, unwieldy and even frightening.
MORE FROM THE LAB: Sign up for our weekly newsletter
A Michigan Medicine vascular surgeon wants to give patients more control.
The vehicle? A values clarification tool that allows them to play a greater role in the decision-making.
Matthew Corriere, M.D., an associate professor of surgery who specializes in peripheral artery disease (PAD), says patient-friendly apps could be the difference maker as clinicians move toward patient-centered care.
Which is why Corriere designed one for the population he treats.
"For a notoriously complicated disease like PAD, there are sometimes multiple different directions you can go," Corriere says. "It's important to reach a shared understanding about what the patient wants to get out of treatment so we can find the right treatment for each person."
Corriere, who served as co-author for the American Heart Association's 2016 PAD guidelines, has piloted the My Treatment Values app in 100 PAD patients and presented on patient desires to share treatment decisions.
He explains why he's a firm believer in going digital.
Why did you create an app?
Corriere: PAD is an inherently complicated diagnosis with no one treatment path. There's a lot to discuss with patients and their families, and I wanted a way to improve trust and be sure we're organizing care plans around the need of the patients.
I found an app was an easy way to enhance this interaction. I tell my patients that this facilitates us figuring out what's important to them and then making a decision together. The patient really may not know what they care about at the beginning, so it's up to us to help.
Much like web-based marketing, I wanted to use an app to show patients different treatment options like different products — and then quantify those preferences to learn more about the patient.
As we move forward, I believe patients will start demanding this sort of thing.
How does your app work?
Corriere: A staffer would hand the tablet to the patient at check-in, and the patient can do the survey before meeting with their doctor. The app presents a series of choices to maximize trade-offs. For example, a patient would evaluate durability versus risk and type of treatment versus symptomatic response.
The patient might also be more honest about some things if they have the option to address them from behind a screen, such as whether they'll be compliant about exercise. When the clinic visit starts, the patient's responses would already be there to help the discussion.
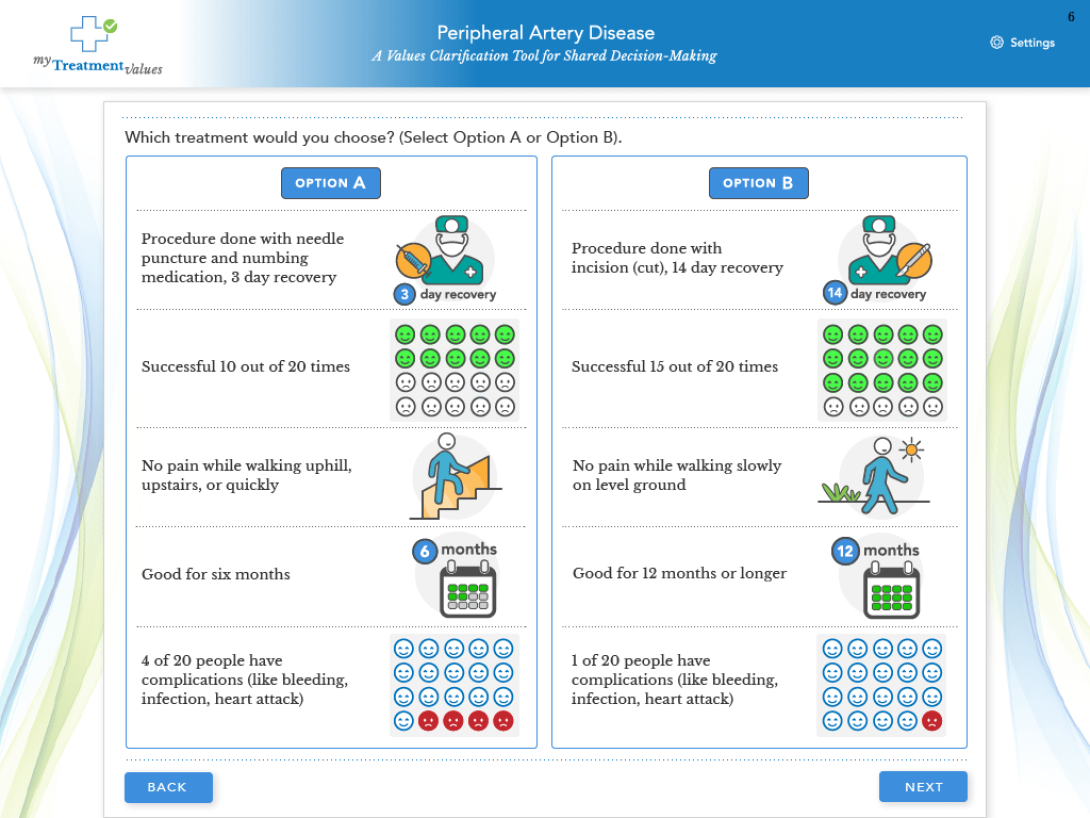
What makes this type of platform different from a regular clinic visit?
Corriere: The values systems that patients rely upon to make decisions are often subconscious and deeply personal, but having the patient spend a few minutes weighing different trade-offs in advance helps bring their priorities to the forefront. Patients who piloted the app tell me they realized what was important to them as they went through the cards.
Then, during the clinic visit, we start with an idea of what the patient cares about. With such a complicated disease, having this extra information at the start of a clinic visit is really helpful.
Patients tell us they want input in their care, and a tool like ours provides a platform to elicit their opinions, quantify them and then apply this information to help design a treatment plan consistent with their values — whether that's an aspirin regimen, a stent or bypass surgery, or another option. It's how I would want to be treated.
What's next?
Corriere: We hope to bring the app into the clinical environment to help PAD providers everywhere enhance their patient-centered care. Right now, we're looking at how we might improve the tool, including making sure the information shown to patients is easily interpretable.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





