A newly launched multicenter study analyzes the use of emergency mechanical circulatory support among critically ill children with cardiovascular conditions.
9:55 AM
Author |
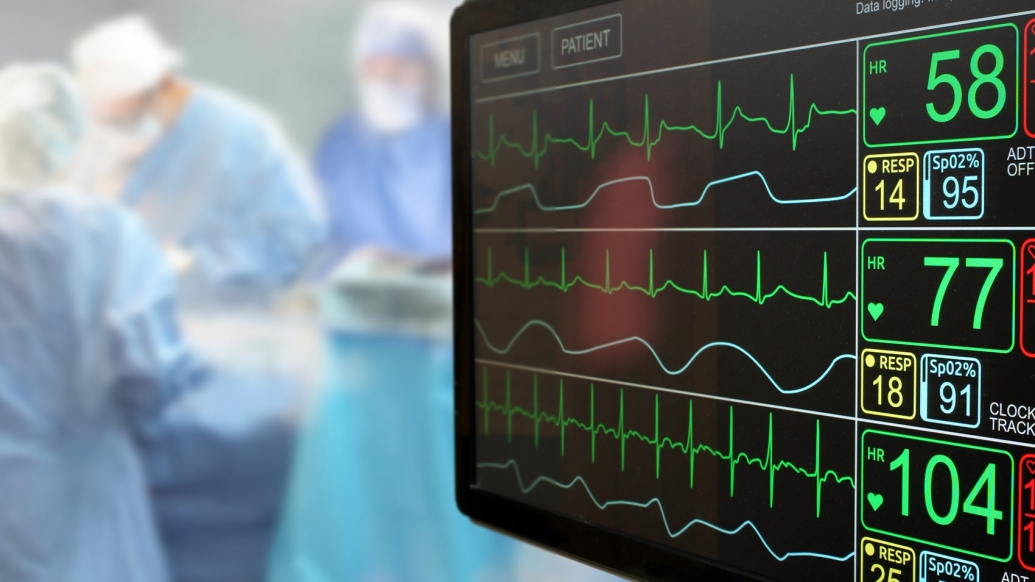
Researchers have launched a multicenter study to better understand and improve outcomes for children with cardiovascular disease who are critically ill and require emergency mechanical circulatory support.
MORE FROM THE LAB: Subscribe to our weekly newsletter
The study analyzes data from 23 hospitals across the country and their use of extracorporeal membrane oxygenation (ECMO) in children cared for in the cardiac intensive care unit. Morbidity and mortality rates remain exceptionally high for children with cardiovascular disease requiring ECMO to support their heart and lungs.
The study was presented as a featured abstract at the 2017 American College of Cardiology Scientific Session in Washington, D.C. The research was performed by the Pediatric Cardiac Critical Care Consortium (PC⁴), the University of Michigan-led multicenter quality improvement and research collaborative geared toward improving pediatric cardiac critical care outcomes.
"We need to know more about the outcomes of these treatments and how those outcomes vary across hospitals. This will help us learn how to best provide care to children who need ECMO support and how to counsel families about this therapy," says the study's senior author, Michael Gaies, M.D., a pediatric cardiologist at U-M's C.S. Mott Children's Hospital and the executive director of PC⁴.
"The use of ECMO in critically ill children with cardiac disease is rare, but the risk of mortality is much too high. There may be opportunities to improve these outcomes by understanding the practices of top-performing hospitals that either avoid ECMO altogether or achieve the best results for patients who do require this therapy."
An estimated 50 to 60 percent of children with cardiac disease sustained by ECMO in the cardiac intensive care unit die every year. Complications associated with ECMO include bleeding, infections and brain injury, along with high cost.
The study has identified several high-risk subgroups to target for quality initiatives within medical and surgical patients. Researchers also found that ECMO utilization rates after cardiac surgery differ significantly across hospitals, with some hospitals using ECMO much less and others much more frequently than would be expected after surgery.
Prior to this study, the outcomes of ECMO therapy had not been fully described in a population of patients with nonsurgical cardiovascular disease, and the differing use across hospitals after surgery has not been previously reported.
Gaies says hospitals' ECMO use in this group of pediatric patients may be an indication of surgical quality, but it requires further investigation. Researchers expect to report more on these findings later this year.
"Our goal is to provide a benchmark of performance for pediatric cardiac surgical programs that helps to inform and drive quality improvement initiatives," he says. "We will continue to explore variation across hospitals in ECMO use and quality of care to identify best practices that can be disseminated across the collaborative."
The abstract was presented at the ACC session Sunday by lead author Marissa Brunetti, M.D., of the Children's Hospital of Philadelphia.
Since its establishment in 2009, PC⁴ has grown to include over 30 participating institutions across the U.S. and Canada

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!