A recent survey found that a majority of doctors who are not foot specialists don’t know enough about a rare form of foot damage, which can lead to significant disability in patients.
1:00 PM
Author |
Diabetes can have several complications, including one common side effect: foot damage. Although some types are common, others are rarer.
Among the lesser-known conditions is Charcot neuroarthropathy.
MORE FROM THE LAB: Subscribe to our weekly newsletter
"It is a rare foot condition that can cause significant deformity, disability and may lead to ulcerations and infections if it is not caught early in the disease process," says Brian Schmidt, D.P.M., clinical instructor in internal medicine and member of the podiatry team at Michigan Medicine.
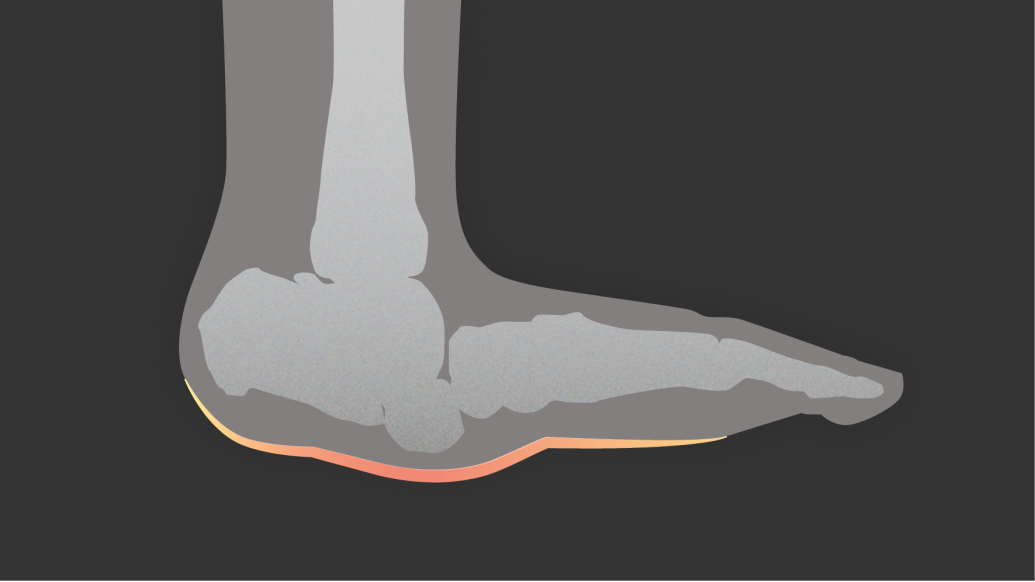
Commonly known as a Charcot foot and/or ankle, the effects can be debilitating.
"The joints of the foot break down, with fracture and dislocation, leading to a rocker bottom foot deformity over time," Schmidt says. "People with peripheral neuropathy are at risk of developing this condition, and today this condition is most commonly seen in patients with diabetes mellitus. However, any patient with peripheral neuropathy is at risk."
Many doctors, however, aren't up to speed on the matter.
Schmidt is the lead author on a new study, published in Clinical Diabetes and Endocrinology, that investigated how much non-foot-specialist clinicians know about the condition in an effort to understand how to better focus future educational forums on the topic.
Of the 400 endocrinologists, internal medicine physicians and family medicine physicians who responded to a survey, more than two-thirds of respondents — 67.6 percent — described themselves as having poor or complete lack of knowledge of Charcot neuroarthropathy. Researchers also investigated how referring physicians treat the condition if they encounter it.
Schmidt explains what the results mean for fellow clinicians:
Why is it so important for physicians to know about Charcot neuroarthropathy, and what types of symptoms should physicians be looking for in patients?
Schmidt: Past studies have demonstrated that referring physicians can misdiagnose Charcot neuroarthropathy up to 95 percent of the time when referring the patient to a foot specialist.
This condition leads to significant morbidity and mortality and is an independent risk factor for limb loss.
SEE ALSO: What Primary Care Providers Should Know About Diabetic Neuropathy
Physicians should be acutely aware of the patient with peripheral neuropathy who presents to their office with sudden onset pain and a red, hot, swollen foot. This condition typically does not have any preceding event leading to a painful foot, and there may or may not be an apparent break in the patient's skin.
What are some ways you recommend fellow physicians learn more about this complication?
Schmidt: There are many comprehensive reviews in multiple peer-reviewed journals, including a review article about the complication. Various foot and ankle societies have a plethora of information about this condition as well. Three sources of information include the American Podiatric Medical Association, Academy of Foot and Ankle Orthopedics, and the American Diabetes Association.
In addition, I am always available by email for questions or concerns.
How might patients potentially benefit from this study?
Schmidt: Patients can potentially benefit from this study by making more physicians aware of this condition. Through education about this condition, it is more likely when a patient presents to a physician with symptoms suggestive of Charcot neuroarthropathy, it will be correctly diagnosed and treated initially. If diagnosed early, many of the untoward complications can be avoided or managed effectively.
Why is it important to study this complication?
Schmidt: Although it's a rarer complication, I see this condition on a daily basis and in various stages with significant consequences. The effects of the condition are devastating and negatively impact a patient's life. I find that patients who have this diagnosis often don't receive the care they need initially and this leads them down a road full of complications. Rather than treat the symptoms and sequelae of disease, I hope to improve diagnosis of this condition, leading to less complications over time.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!